By Dr. Ara Deukmedjian, MD
Board-Certified Neurosurgeon, Deuk Spine Institute
Medically reviewed on April 1, 2026
Medical Disclaimer: This content is for educational purposes only and does not constitute medical advice. Individual results may vary. Always consult with your healthcare provider about your specific condition and treatment options.
Key Points
✓ Disc protrusion is one of the most common forms of disc herniation, affecting millions of Americans and often resolving on its own within six to eight weeks with conservative care.
✓ There are three main locations where protrusions occur: central, foraminal, and paracentral. Each affects the spine differently and produces distinct symptoms.
✓ Diagnosis requires a full clinical evaluation including MRI, which remains the gold standard for visualizing disc abnormalities and nerve compression.
✓ Conservative treatment, including physical therapy, rest, and medications, is appropriate for most patients and is effective in the majority of cases.
✓ Surgery is reserved for cases where conservative treatment has failed after several months, or when symptoms are severe and neurologically debilitating.
✓ A 2025 systematic review published in Neurospine confirmed that conservative care should be the first-line approach for most patients before surgical intervention is considered.
✓ Preventive strategies such as core strengthening, proper posture, and avoiding repetitive heavy lifting significantly reduce the risk of developing disc protrusion.
✓ Deuk Laser Disc Repair® is designed to target inflamed disc tissue through a small incision while preserving normal spine structure and motion.

What Is Disc Protrusion?
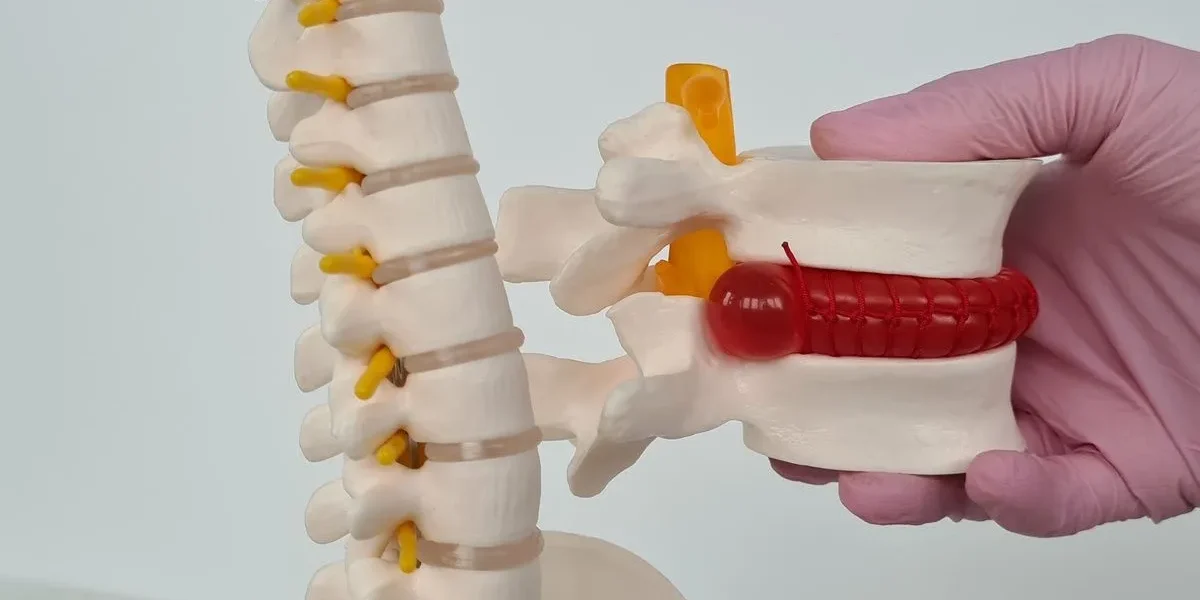
Think of a spinal disc as a jelly-filled pastry. The outer layer is a tough, fibrous ring called the annulus fibrosus, and the inner core is a soft, gel-like substance called the nucleus pulposus. This inner material acts as a shock absorber between each of the vertebrae in your spine. When the inner gel pushes outward against the outer wall of the disc without breaking through it, that is a disc protrusion. If the outer wall tears completely and the inner material escapes, it becomes a herniated disc or extrusion. If a fragment breaks free entirely, that is called disc sequestration.
Disc protrusion is classified as a type of disc herniation, but it is an important distinction: in a protrusion, the displaced disc material remains connected to the parent disc. The base of the protrusion is wider than the protruding portion, which distinguishes it radiologically from an extrusion.
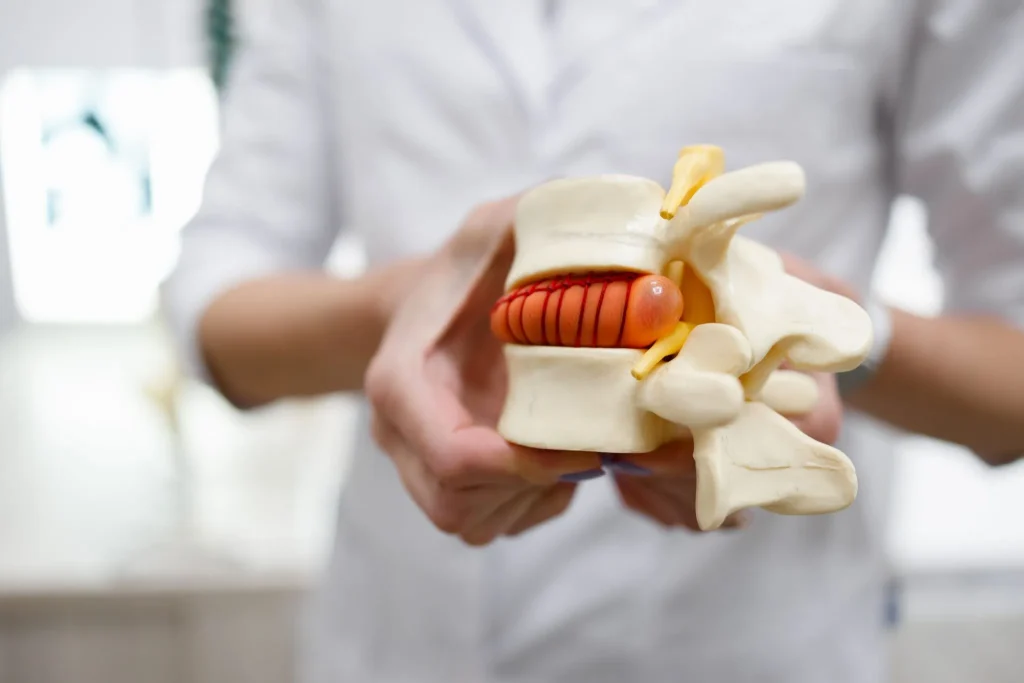
Types of Disc Protrusion by Location
Disc protrusions are further categorized by where they push into the spinal canal:
Central Disc Protrusion
This occurs when the disc pushes directly into the center of the spinal canal. It can compress the spinal cord itself or cause bilateral symptoms affecting both sides of the body. Central protrusions carry a higher risk of serious neurological consequences if left untreated.
Foraminal Disc Protrusion
The foramen is the opening through which nerve roots exit the spinal cord and branch outward. A foraminal protrusion advances into this opening, compressing an exiting nerve root and causing pain, numbness, or weakness that radiates along the nerve’s path, often into the arm or leg.
Paracentral Disc Protrusion
This is the most common type. Paracentral protrusions occur in the space between the central canal and the foramen. They can compress nerve roots at the level of the disc, producing unilateral symptoms such as radiating leg pain, known as sciatica, or arm pain depending on the spinal level affected.
Symptoms of Disc Protrusion
Symptoms depend on the location and severity of the protrusion, as well as whether any nerve structures are being compressed. Common presentations include:
- Localized back or neck pain at the level of the affected disc
- Radiating pain that travels down the leg (sciatica) or arm (cervical radiculopathy)
- Numbness or tingling in the hands, feet, or along a limb
- Muscle weakness in the arms or legs
- Reduced range of motion or stiffness in the spine
- Pain that worsens with sitting, bending, coughing, or sneezing
It is worth noting that not all disc protrusions cause pain. Research has consistently shown that spinal disc abnormalities are frequently visible on imaging in people who have no symptoms at all. This means a disc protrusion on an MRI report does not automatically translate into a need for surgery or even aggressive treatment.
What Causes Disc Protrusion?
Disc protrusions can arise from a combination of degenerative changes, physical demands, and lifestyle factors. The most common contributing causes include:
Age-Related Disc Degeneration
All structures of the spine change with age. Intervertebral discs begin losing water content and flexibility as early as the third decade of life. As the nucleus pulposus becomes drier and less resilient, the annulus fibrosus is more likely to weaken and allow the inner material to push outward. This is why disc protrusion becomes increasingly common after age 35.
Mechanical Stress and Repetitive Loading
Occupations or activities that involve frequent heavy lifting, twisting, or bending place cumulative stress on the discs over time. Research shows that workers in physically demanding industries face an elevated risk of disc herniation. Even sedentary workers are not immune: prolonged sitting at a desk, especially with poor posture, creates sustained compressive pressure on the lumbar discs.
Acute Injury
A single high-impact event, such as a car accident, a sports collision, or a fall, can generate sufficient spinal loading to protrude a disc that was previously healthy. Acute disc protrusions following trauma tend to produce more immediate and severe symptoms than those that develop gradually.
Genetic and Lifestyle Factors
Genetics play a role in how quickly discs degenerate. Obesity increases compressive forces on the lumbar spine, and smoking impairs the blood supply to disc tissue, accelerating dehydration and degeneration. Lack of core muscle strength reduces spinal stability and places greater demands on the discs to bear load.
How Is Disc Protrusion Diagnosed?
A thorough and accurate diagnosis is essential before any treatment decision is made. At Deuk Spine Institute, diagnosis begins with a complete clinical evaluation that includes a review of your medical history, a discussion of your symptoms, and a physical examination of your range of motion and neurological function.
Physical Examination
Your physician will assess your posture, reflexes, muscle strength, and sensation to identify any neurological deficits. Specific tests, such as the straight leg raise test for lumbar nerve root involvement, help pinpoint the affected spinal level.
MRI Imaging

Magnetic resonance imaging is the gold standard for visualizing disc protrusions. MRI provides detailed, high-resolution images of both the bony structures and soft tissues of the spine, allowing clinicians to identify the exact location of the protrusion, the degree to which it encroaches on the spinal canal or neural foramen, and whether any nerve roots are being compressed. It can also reveal associated inflammation, annular tears, and other contributing factors.
CT Scan and X-Ray
While X-rays do not show disc tissue directly, they are useful for evaluating bone alignment, disc space height, and any signs of instability. CT scans can provide additional detail about bone anatomy and calcified disc material when MRI findings are inconclusive.
At Deuk Spine Institute, we offer a free MRI review so that patients can receive an expert assessment of their imaging and a clear explanation of what their findings actually mean for their treatment options.
Conservative Treatment Options
The majority of disc protrusion cases improve with conservative, non-surgical care. A 2025 systematic review published in Neurospine confirmed that conservative treatment should be the established first-line approach for lumbar disc herniation before any surgical intervention is considered.
A 2025 systematic review published in Neurospine confirmed that conservative treatment should be the established first-line approach for lumbar disc herniation before any surgical intervention is considered. Most disc protrusion situations improve within six to eight weeks with appropriate conservative management. 1
Rest and Activity Modification
A short period of rest is often the starting point, particularly in the acute phase when inflammation and pain are at their peak. However, prolonged bed rest is generally not recommended. Gradual return to gentle movement is encouraged as soon as tolerable, as activity promotes circulation and healing.
Physical Therapy and Exercise
Structured physical therapy is among the most effective conservative interventions available. A 2025 meta-analysis published in Frontiers in Medicine reviewed eight randomized controlled trials encompassing 611 patients and found that exercise therapy significantly improved pain scores, disability index scores, range of motion, and quality of life in patients with lumbar disc herniation. 2 The analysis concluded that exercise therapy enhances core muscle strength and lumbar stability, making it a highly effective and accessible treatment option.
Core stabilization exercises strengthen the paraspinal and abdominal muscles that support the spine. A strong core reduces the mechanical load placed on the discs during daily activities. Patients who build consistent core strength before problems arise are far less likely to develop significant disc issues or to experience reinjury after recovery.
Medications
Nonsteroidal anti-inflammatory drugs (NSAIDs), muscle relaxants, and in some cases oral corticosteroids can help control pain and reduce inflammation during the acute phase. These are used to improve a patient’s ability to participate in physical therapy and daily function, not as standalone long-term solutions.
Massage Therapy

Therapeutic massage can reduce muscle tension, improve blood flow, and provide meaningful pain relief in conjunction with other conservative treatments. It is typically used as a complementary therapy alongside physical therapy rather than as primary treatment.
Interventional Pain Management
When pain is severe enough to prevent participation in rehabilitation, interventional approaches such as epidural steroid injections can provide temporary relief. A 2024 systematic review and meta-analysis published in Frontiers in Neurology found that epidural steroid injections can provide meaningful symptom relief for sciatica secondary to lumbar disc herniation, particularly in the short term. 4 By reducing nerve root inflammation, injections can create a window of pain relief that allows patients to engage more effectively in rehabilitative exercise.
Spontaneous Resorption: The Body’s Own Healing Process
One of the most encouraging aspects of disc protrusion is the body’s capacity for natural healing. A comprehensive 2025 review published in Frontiers in Medicine examined the biological mechanisms behind lumbar disc herniation reabsorption, in which herniated disc tissue shrinks naturally without surgery. 5 The review found that inflammatory responses and macrophage activation play key roles in symptom relief during the natural healing process, providing a biological explanation for why most disc protrusion cases improve with time and conservative care.

When Is Surgery Necessary for Disc Protrusion?
Surgery is not the first option for disc protrusion, and it should not be. However, there are clear clinical situations in which surgical intervention becomes appropriate and necessary. Learn about the different options to treat your chronic back pain.
According to clinical guidelines reviewed in a 2025 systematic review in Neurospine, surgery should be considered when:
- Conservative treatment has been pursued comprehensively for several months without adequate relief
- Symptoms are severe and significantly impair daily function, work, or quality of life
- Progressive neurological deficits are present, such as worsening weakness, numbness, or loss of bladder or bowel control
- Cauda equina syndrome is suspected, which is a medical emergency requiring immediate surgical decompression
A 2025 systematic review and meta-analysis examined surgical versus nonsurgical management for lumbar disc herniation and noted that patients with longer symptom duration before surgery tended to have worse postoperative outcomes. 6 This reinforces the importance of not unnecessarily delaying surgery once conservative care has clearly failed.
Micro Lumbar Discectomy
The most established surgical treatment for lumbar disc protrusion is the micro lumbar discectomy. This minimally invasive outpatient procedure involves removing only the protruding portion of the disc that is compressing the nerve. It is performed through a small incision and uses specialized magnification to minimize trauma to surrounding tissues. Most patients are able to walk the same day and return to normal activities relatively quickly.
Deuk Laser Disc Repair (DLDR)
At Deuk Spine Institute, we offer Deuk Laser Disc Repair® (DLDR), an advanced minimally invasive endoscopic procedure that addresses disc problems while preserving the spine’s natural structure and motion. Unlike fusion procedures, DLDR requires no screws, rods, or metal implants. It removes only the inflamed and damaged portion of the disc while leaving healthy disc tissue intact. Patients typically experience immediate pain relief and can return to activity within days, not months. DLDR has been documented in peer-reviewed medical literature with a 99.6% success rate in eliminating disc-related pain and zero surgical complications.
Importantly, starting with the least invasive surgical approach preserves future options. If a minimally invasive procedure does not provide complete relief, more extensive surgery remains available. However, beginning with a highly destructive procedure such as spinal fusion permanently limits future treatment flexibility.
Preventing Disc Protrusion
While disc degeneration is a natural part of aging, there are evidence-based strategies that significantly reduce your risk of developing a symptomatic disc protrusion or experiencing recurrence after recovery.
Build Core Strength Before Problems Arise
The most effective prevention strategy is a proactive one. Core-strengthening exercises, including Pilates-based movements, planks, bridges, and bird-dog progressions, build the muscular foundation that offloads compressive pressure from the discs. Do not wait until you feel pain to start strengthening your core. Make it a consistent habit.

Practice Safe Lifting and Movement
Reducing repetitive twisting, bending, and heavy lifting significantly reduces disc stress. When lifting is necessary, use proper mechanics: keep the load close to your body, bend at the hips and knees rather than the waist, and avoid twisting while bearing weight. Lifting a 50-pound object can place 500 or more pounds of pressure on lumbar discs, so technique matters enormously.
Maintain a Healthy Weight
Excess body weight increases compressive forces on the lumbar spine, accelerating disc degeneration. Achieving and maintaining a healthy body weight through a balanced diet and regular low-impact exercise reduces the mechanical burden on your discs and supports long-term spinal health.
Prioritize Ergonomics
If your work involves prolonged sitting, invest in a chair that supports the natural lumbar curve, position your monitor at eye level, and take regular breaks to stand and move. Sustained sitting positions, especially with poor posture, place continuous compressive pressure on the lumbar discs and accelerate the degeneration process over time.
Avoid Smoking
Smoking reduces blood supply to the intervertebral discs and accelerates the disc dehydration that leads to protrusion. Quitting smoking is one of the most impactful steps you can take for long-term spinal health.
Stay Active Consistently
Regular low-impact activity, such as walking, swimming, or cycling, keeps the discs hydrated, maintains spinal flexibility, and strengthens the supportive musculature around the spine. Research on running exercise has even found that long-distance runners show better disc hydration compared to sedentary individuals, suggesting that appropriate loading has anabolic effects on disc tissue.

When to Seek Medical Attention
If you or a loved one is experiencing back or neck pain that radiates into the arms or legs, numbness, tingling, or muscle weakness, it is time to seek a professional evaluation. These symptoms suggest nerve involvement and require imaging to assess the underlying cause.
Seek emergency care immediately if you experience sudden loss of bladder or bowel control, saddle anesthesia (numbness in the groin and inner thighs), or rapidly progressive bilateral leg weakness. These are signs of cauda equina syndrome, which is a surgical emergency.
At Deuk Spine Institute, we offer a free consultation and MRI review with Dr. Ara Deukmedjian, a board-certified neurosurgeon. Our goal is to help you understand your diagnosis accurately and explore all available options, from conservative care to the most advanced minimally invasive surgical techniques available. We believe in empowering patients to make informed decisions about their own spinal health.

Frequently Asked Questions
-
Is disc protrusion the same as a herniated disc?
Disc protrusion is a type of disc herniation, but they are not identical. A protrusion is a contained herniation where the disc material pushes outward but the outer fibrous ring remains intact. In a true extrusion, that outer layer ruptures and material escapes. Disc sequestration occurs when a fragment completely separates. Protrusions are generally less severe than extrusions or sequestrations, though any of these conditions can cause significant nerve compression and symptoms.
-
How long does disc protrusion take to heal?
Most disc protrusions improve significantly within six to eight weeks with appropriate conservative treatment, including rest, physical therapy, and anti-inflammatory medications. Some patients experience full resolution of symptoms, while others may continue to have intermittent discomfort that is manageable with activity modification and exercise. Complete healing timelines vary based on the severity of the protrusion, the patient’s age and overall health, and their adherence to rehabilitative care.
-
Can disc protrusion come back after treatment?
Yes, recurrence is possible, particularly if the underlying risk factors, such as weak core muscles, poor posture, or continued heavy lifting, are not addressed. Patients who complete a structured rehabilitation program, build consistent core strength, and adopt ergonomic habits significantly reduce their risk of recurrence. For patients who undergo surgery, recurrent protrusion at the same or adjacent level can occur, which is one reason why minimally invasive approaches that preserve disc tissue are preferred over more destructive procedures.
-
Do I need surgery for a disc protrusion?
Most patients with disc protrusion do not need surgery. Conservative treatment is effective for the majority of cases, and the body has a natural capacity to resorb and reduce disc protrusions over time. Surgery becomes appropriate when conservative care has failed after several months, when neurological symptoms are progressing, or when pain is severe enough to prevent any meaningful daily function. If you have been told you need surgery, we encourage you to get a free MRI review at Deuk Spine Institute to understand all of your options before making a decision.
Sources
1. Jin H, Lopez AM, Garza Romero F, et al. A systematic review of treatment guidelines for lumbar disc herniation. Neurospine. 2025;22(2):389-402.
2. Du S, Cui Z, Peng S, et al. Clinical efficacy of exercise therapy for lumbar disc herniation: a systematic review and meta-analysis of randomized controlled trials. Front Med (Lausanne). 2025;12:1531637.
3. Lumbar disc herniation reabsorption: a review of clinical manifestations, mechanisms, and conservative treatments. Front Med (Lausanne). 2025;12:1633762.
4. Efficacy of epidural steroid injection in the treatment of sciatica secondary to lumbar disc herniation: a systematic review and meta-analysis. Front Neurol. 2024;15:1406504.
5. Indications for surgery versus conservative treatment in the management of lumbar disc herniations: A systematic review. ScienceDirect. 2025.
6. Review of recent treatment strategies for lumbar disc herniation focusing on nonsurgical and regenerative therapies. J Clin Med. 2025;14(4):1196.