Procedure Not Recommended
Temporary Relief with Real Risks
⚠️ While Deuk Spine Institute can perform Epidural Steroid Injections, we do not recommend them.
This page explains why — learn the risks before consenting to this procedure.
UNDERSTANDING THE PROCEDURE
While there are legitimate medical reasons, financial incentives often influence recommendations from pain management doctors and spine surgeons.
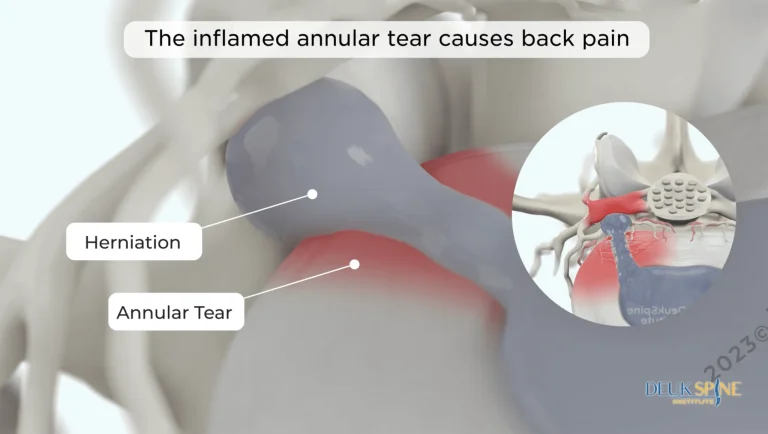
Nerve root dysfunction from compressed or pinched nerves. However, ESIs only temporarily mask the inflammation without addressing the structural cause.
Pain radiating down the leg to the foot from compressed nerves. Steroid injections may numb the pain temporarily but leave the herniated disc untreated.
Poly radiculopathy from compressed nerves. A serious condition that requires actual treatment — not temporary steroid relief.
General back pain from various spinal conditions. ESIs are not an accepted treatment for back pain and provide only temporary, partial relief at best.
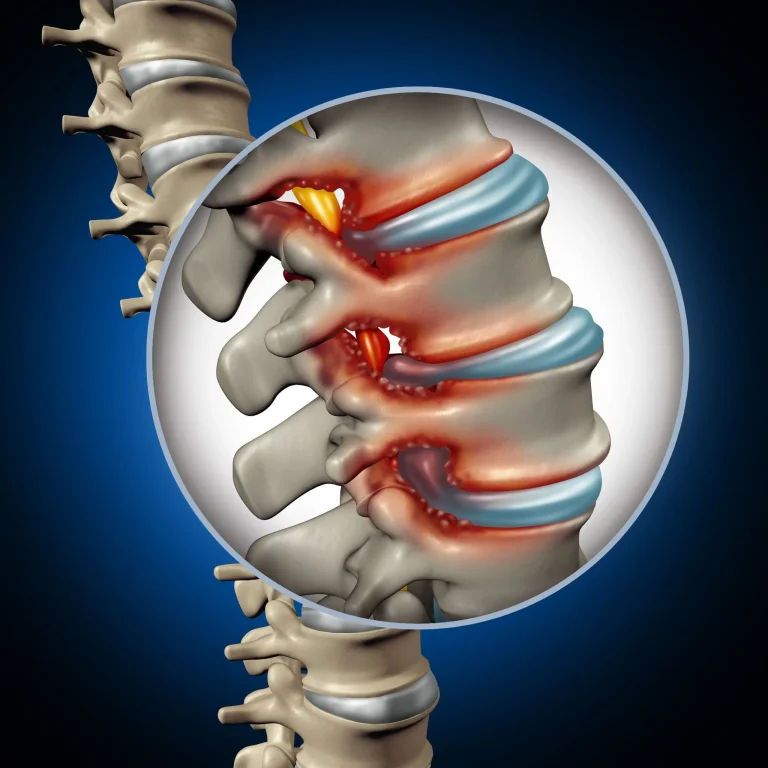
Narrowing of the spinal canal causing nerve compression. Steroid injections cannot widen the canal — stenosis will worsen without proper treatment.
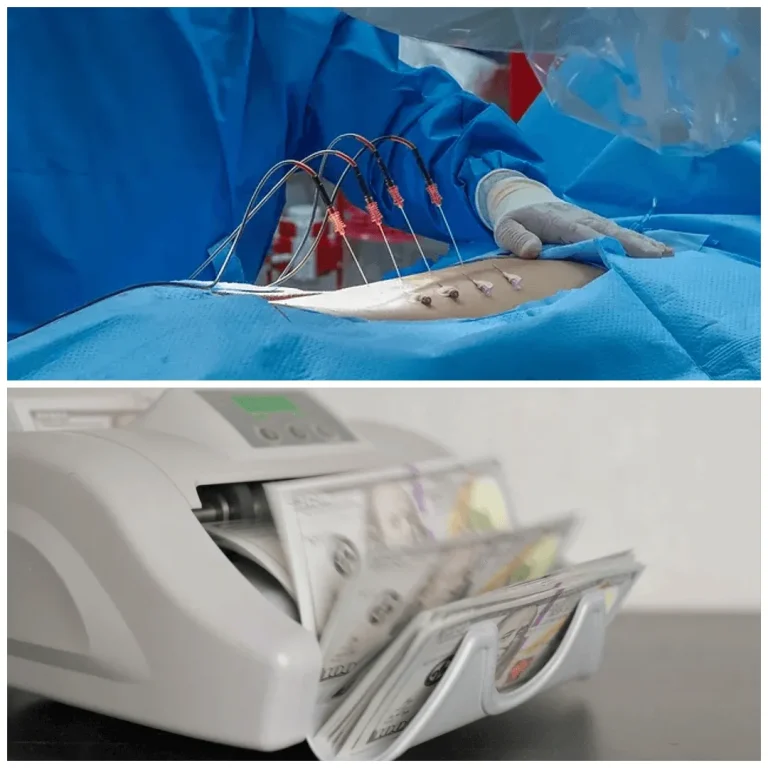
A quick procedure that takes minutes. Doctors can perform 10-20 per day at 00-,000 each, generating massive daily revenue.
An additional ,000-,000 per injection for facility fees and fluoroscopic imaging guidance, on top of the physician fee.
Relief is temporary by design. Patients return every 3-6 months indefinitely, creating a predictable, recurring revenue stream.
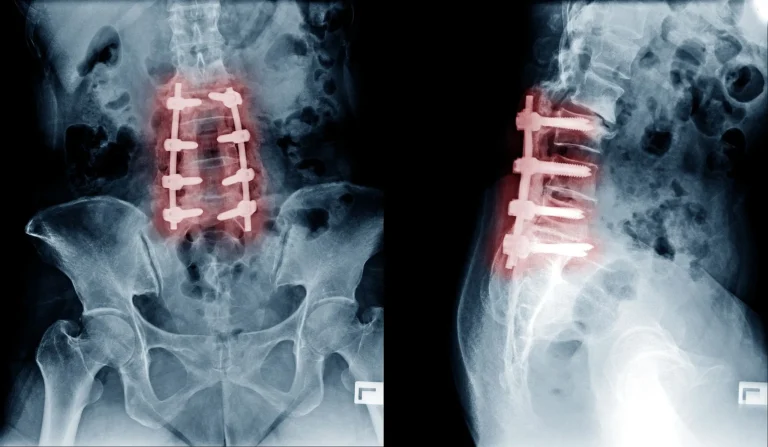
When injections inevitably fail, surgeons recommend expensive spinal fusion surgery — a procedure that is often unnecessary.
THE INJECTION PROCESS
Images below contain medical imagery and procedural evidence. Viewer discretion is advised.
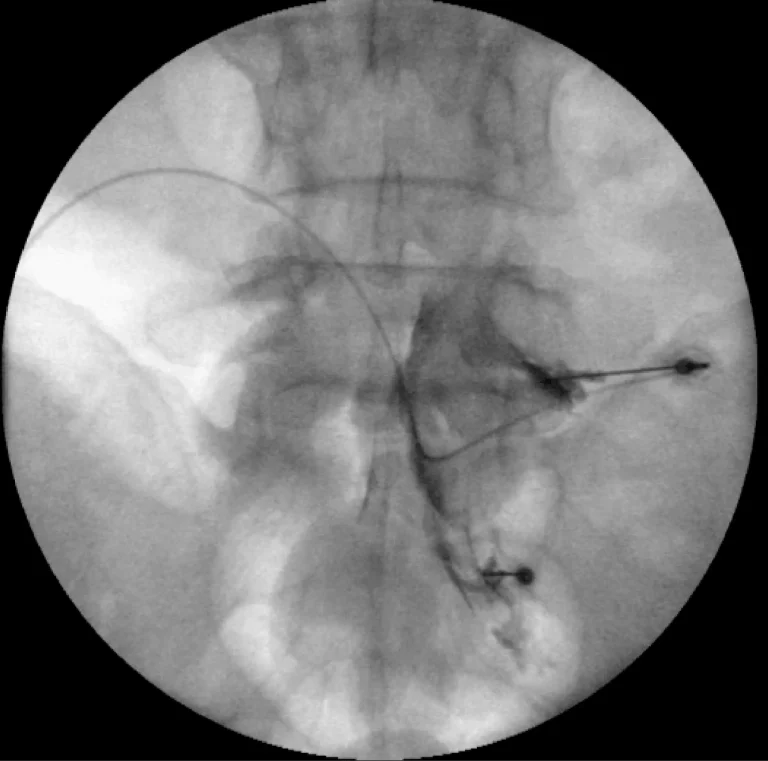
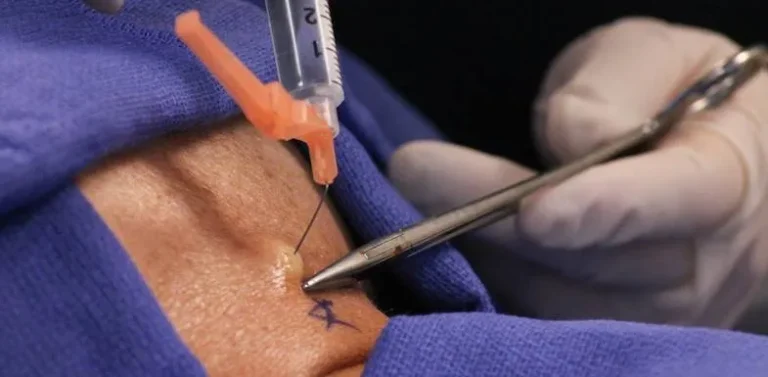
Fluoroscopic (X-ray) guidance is used to visualize the spine and guide needle placement in real time.
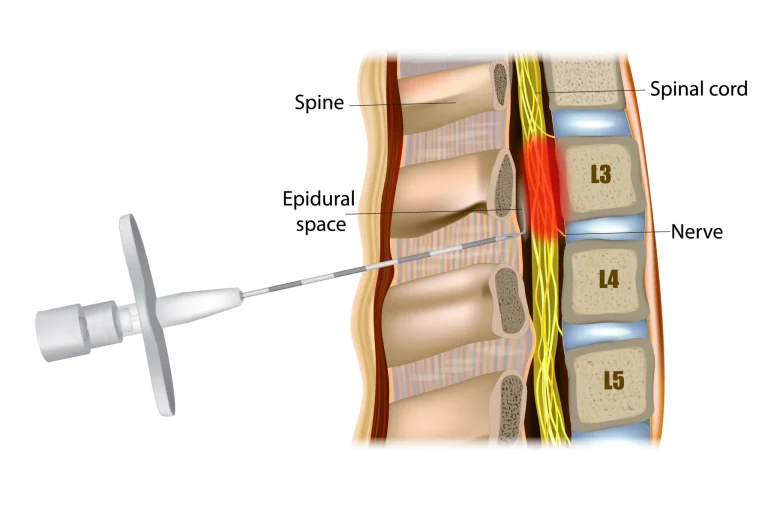
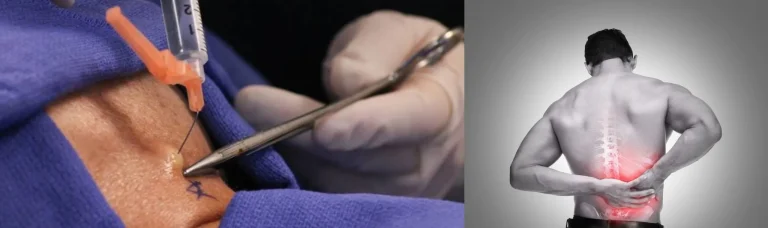
A needle is directed into the spinal canal near the source of inflammation using continuous X-ray monitoring.
Steroid medication is injected into the epidural space around the nerve roots to temporarily reduce inflammation.
CRITICAL RISKS
11 documented reasons with supporting images and medical evidence.
Images below contain medical imagery and procedural evidence. Viewer discretion is advised.

DOCUMENTED COMPLICATIONS
Images and videos below contain real surgical procedures and medical imagery.
Needle contact with nerve roots can cause permanent damage, weakness, or numbness in extremities.
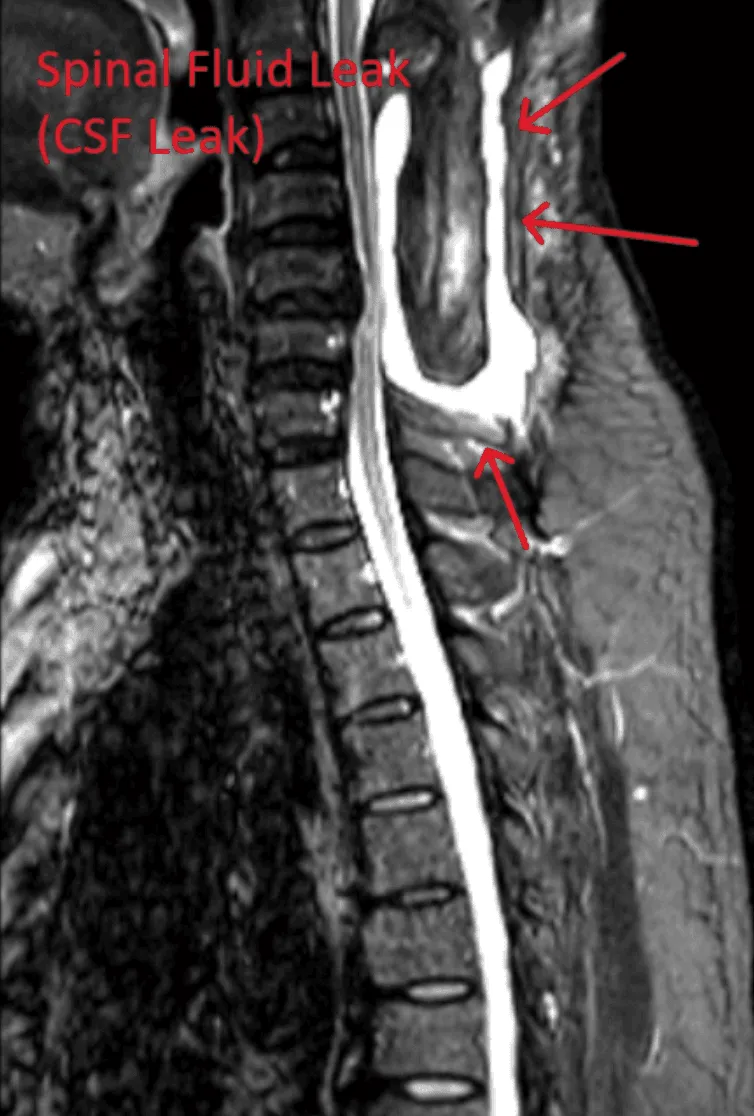
Dural puncture from the needle causes cerebrospinal fluid leaks, leading to severe headaches and potential complications.
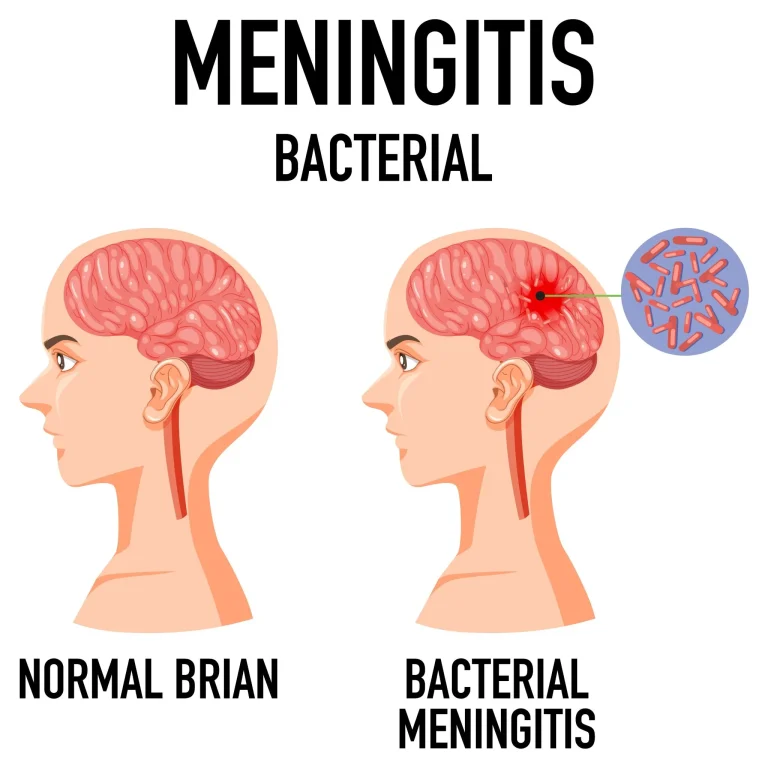
Epidural abscess or meningitis from bacteria introduced during injection into the spinal canal.
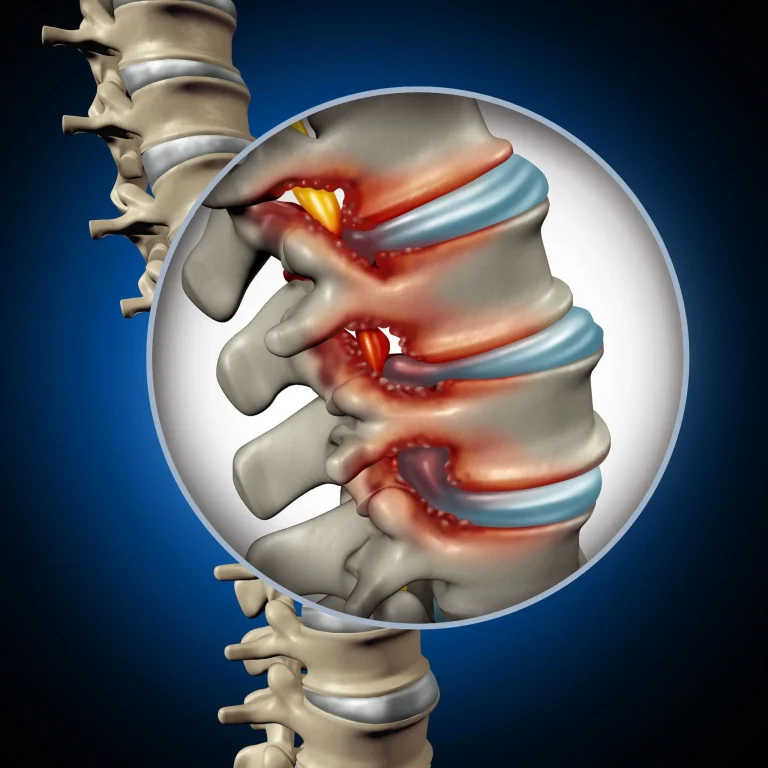
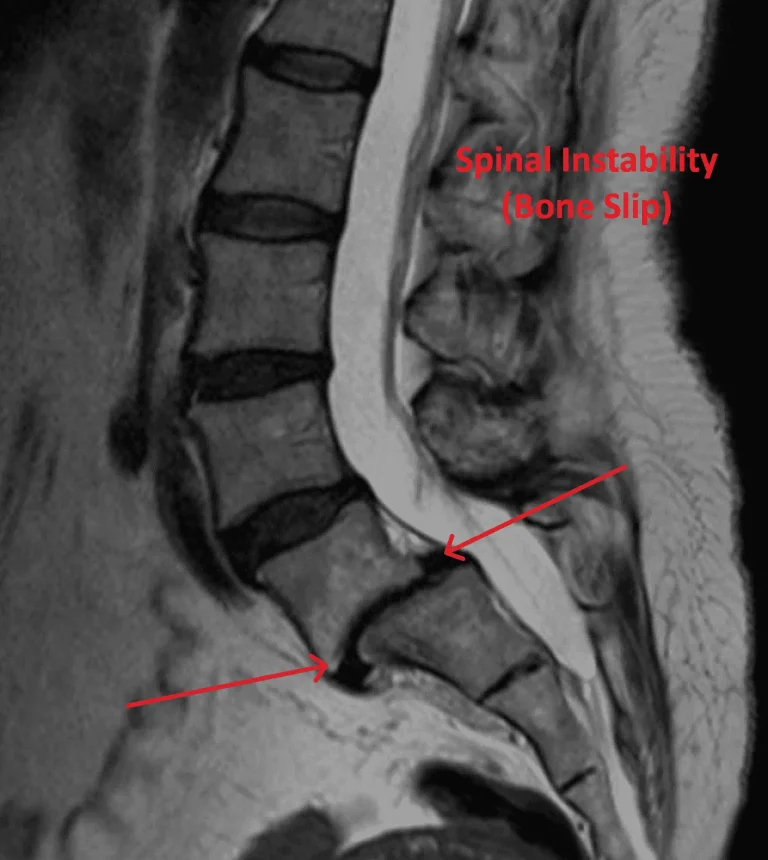
Spinal stenosis is not treated by injection and continues to worsen, requiring actual intervention.
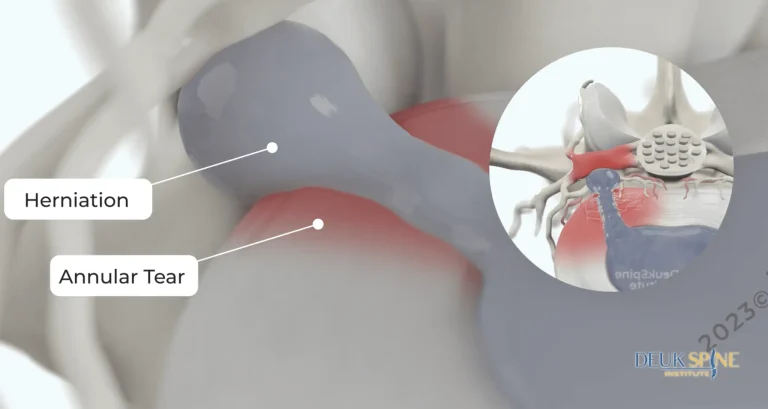
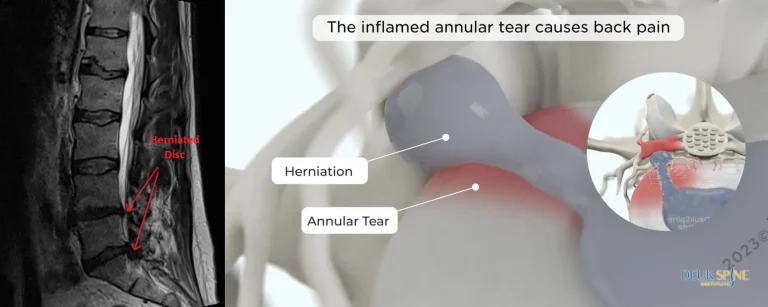
The herniated disc causing pain is left completely untreated, continuing to compress nerves and degenerate.

Rare but documented cases of paralysis from needle-induced spinal cord or nerve damage during injection.

Extremely rare but documented fatalities from epidural abscess, meningitis, or vascular injection complications.
WHAT WE RECOMMEND INSTEAD
Instead of masking pain with temporary steroid injections, Deuk Spine Institute offers three proven procedures that treat the actual source of pain: Deuk Laser Disc Repair®, Deuk Piriformis Release, and Deuk Plasma Rhizotomy®.
Laser technology directly repairs the damaged disc — the actual source of pain that steroid injections only temporarily mask.
No more repeat injections every 3-6 months. A single procedure provides long-term pain elimination instead of temporary relief.
Outpatient procedure under light sedation. Walk out the same day — no hospital stay, no intubation, no opioids required.
95% patient satisfaction, 0.01% complication rate, and over 1,300 successful procedures performed by Dr. Deukmedjian.
Feature
Epidural Steroid Injection
Deuk Laser Disc Repair®
Approach
❌ Temporarily masks pain
✅ Treats the source of pain
Duration of Relief
❌ Temporary — weeks to months
✅ Long-term pain elimination
Treatment Target
❌ Injects steroid near nerves
✅ Repairs the damaged disc with laser
Disc Injury
❌ Left untreated
✅ Directly treated
Repeat Procedures
❌ Every 3-6 months indefinitely
✅ Single procedure
Hospital Stay
❌ Outpatient procedure
✅ Outpatient — same day
Recovery Time
❌ 1-3 days of rest
✅ Days
Complication Rate
❌ Nerve damage, paralysis, death risk
✅ 0.01%
Success Rate
❌ Temporary relief, often fails
✅ 95% patient satisfaction
Long-term Outcome
❌ Pain management dependency
✅ Pain elimination
A BETTER ALTERNATIVE
Permanent pain relief. No injections. No steroids. Minimally invasive, outpatient procedure with a 0.01% complication rate and 95% patient satisfaction.
Patient Satisfaction
Complication Rate
Procedure Time