By Dr. Ara Deukmedjian, MD
Board-Certified Neurosurgeon, Deuk Spine Institute
Medically reviewed on March 26, 2026
Medical Disclaimer: This content is for educational purposes only and does not constitute medical advice. Individual results may vary. Always consult with your healthcare provider about your specific condition and treatment options.
Key Points
✓ Chronic back pain is defined as pain lasting 12 weeks or longer. About 20% of people with acute low back pain go on to develop chronic symptoms.
✓ The Global Burden of Disease Study 2021 found that low back pain affected 619 million people worldwide in 2020, and projections suggest over 843 million cases by 2050. 1
✓ There are four primary types of chronic back pain: nerve pain, muscle pain, arthritis pain, and pain from spinal stenosis. Each type may require a different treatment approach.
✓ Annular tears in spinal discs are a leading cause of discogenic back pain. When the nucleus pulposus pushes through a tear, it triggers inflammation and persistent pain.
✓ A 2025 systematic review in The Lancet Rheumatology found that exercise and psychological interventions reduce chronic low back pain intensity at one to two year and two-plus year follow-up. 2
✓ A 2025 network meta-analysis in Frontiers in Public Health identified exercise sessions of 15 to 30 minutes as most effective for improving chronic low back pain outcomes. 3
✓ When conservative treatments fail, minimally invasive procedures like Deuk Laser Disc Repair® offer a 99.6% success rate with no complications in properly selected patients.

What Is Chronic Back Pain?
Chronic back pain is one of the most widespread and disabling medical conditions in the world. It is defined as back pain that persists for 12 weeks or longer, regardless of an initial injury or underlying cause. Without appropriate treatment, chronic back pain can last for months, years, or even decades, steadily eroding a person’s ability to work, move, sleep, and live well.
The scale of the problem is staggering. According to the Global Burden of Disease Study 2021, low back pain affected approximately 619 million people globally in 2020, and researchers project that number will surpass 843 million by 2050. 1 In the United States alone, an estimated 15.4% of the working population reports an average of 10.5 lost workdays per year due to chronic low back pain, amounting to approximately 264 million workdays lost annually.
The consequences extend well beyond physical discomfort. Chronic back pain causes substantial psychological and emotional distress, contributes to anxiety and depression, disrupts sleep, and strains personal relationships. It is also a leading driver of healthcare costs, disability claims, and early retirement worldwide.
Understanding the nature of chronic back pain, including what causes it, what types exist, how it is diagnosed, and what treatment options are available, is the first step toward effective management and, for many patients, lasting relief.
How Acute Back Pain Becomes Chronic
Not all back pain becomes chronic. Acute low back pain, which lasts less than four weeks, resolves on its own in the majority of cases. However, a meaningful subset of patients follow a more difficult trajectory.
A 2024 community-based cohort study published in The Journal of Pain found that approximately 32% of people with acute low back pain had transitioned to chronic low back pain at three months. Of those who had chronic pain at three months, 80.6% continued to have it at six months. 2 Factors associated with a greater likelihood of transitioning included higher pain intensity at onset and a history of frequent acute pain episodes.
Several biological and psychosocial factors influence whether acute pain becomes chronic. These include the severity and location of the initial injury, the presence of psychological stress or anxiety, sleep disturbance, sedentary behavior, obesity, and smoking. Research from the Global Burden of Disease Study 2021 found that occupational factors, smoking, and high body mass index together account for nearly 39% of all years lived with disability from low back pain.
Additionally, emerging neuroscience research has shed light on central sensitization, a process by which repeated pain signals cause the nervous system to become hypersensitive, amplifying pain responses even in the absence of ongoing tissue damage. This mechanism helps explain why some patients continue to experience severe pain long after an initial injury has structurally healed.
The Four Primary Types of Chronic Back Pain
Chronic back pain is not a single condition but a category of conditions with distinct causes, characteristics, and optimal treatments. Correctly identifying the type of chronic back pain is essential for choosing the most effective intervention.

1. Nerve Pain (Radicular Pain)
Nerve pain, also called radicular pain, occurs when a nerve in the spine becomes compressed or chemically irritated. The most common presentation is sciatica, a sharp, shooting, burning, or electric pain that radiates from the lower back down through the buttock and into one leg. This pattern occurs because the sciatic nerve, the largest nerve in the body, exits the lumbar spine and travels down the leg. When a herniated disc, bone spur, or narrowed spinal canal compresses the nerve root, the pain travels along the entire pathway of that nerve.
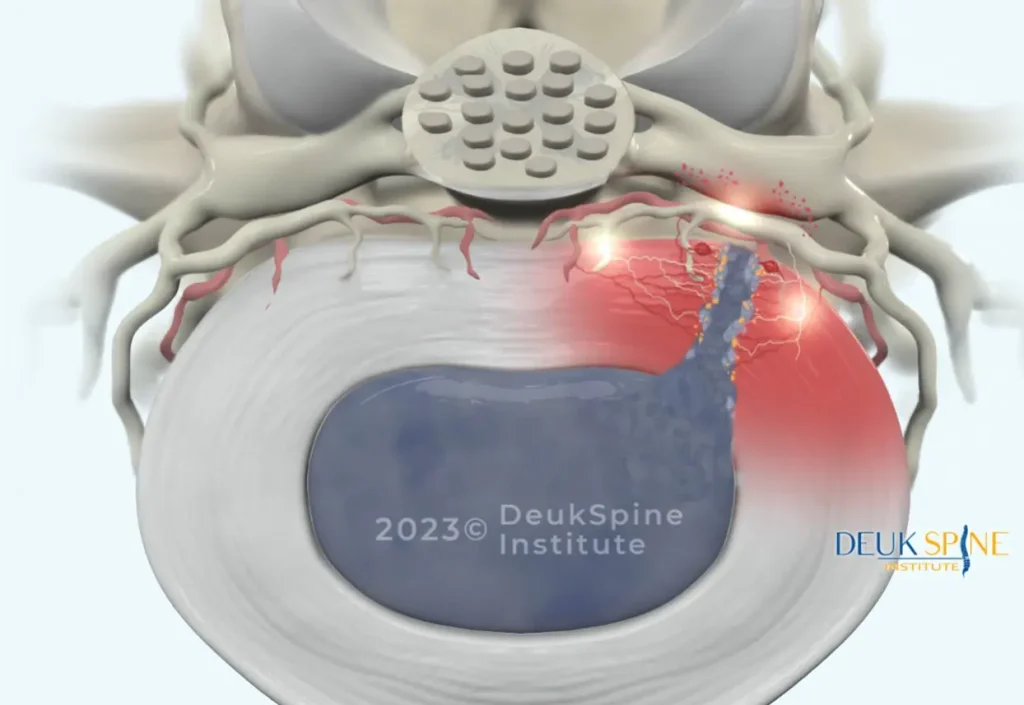
Nerve pain is often described as sharp, stabbing, burning, or like an electric shock. It may be accompanied by numbness, tingling, or muscle weakness in the leg or foot. In severe cases, patients may experience difficulty walking or controlling their bladder or bowel, which require immediate medical attention.
2. Muscle Pain (Myofascial Pain)
Muscle pain, or myofascial pain, results from sustained tension, overuse, micro-tears, or trigger points within the back muscles. It is typically described as a deep, achy, or throbbing discomfort concentrated in the lower or mid-back. Unlike nerve pain, it generally does not radiate down the leg. Prolonged sitting, poor posture, heavy lifting, sudden awkward movements, and emotional stress can all contribute to muscle pain.

3. Arthritis Pain (Facet Joint Pain)
Arthritis pain in the back typically originates from the facet joints, small paired joints located at the back of each vertebra. These joints guide and stabilize spinal movement. With age and wear, the cartilage protecting these joints degrades, leading to inflammation, bone-on-bone friction, and the formation of bone spurs. Facet joint pain is characteristically achy, burning, or stiff, often worse in the morning, after prolonged sitting, or with backward-bending movements. It may refer pain to the buttocks and thighs but rarely extends below the knee.
Facet joint arthritis frequently coexists with disc degeneration, compounding the overall pain burden. Treatment options include anti-inflammatory medications, physical therapy, facet joint injections, and, when appropriate, minimally invasive nerve ablation procedures.
4. Spinal Stenosis Pain
Spinal stenosis occurs when the spinal canal, the hollow channel that houses the spinal cord and nerve roots, narrows due to age-related changes, disc degeneration, or bone spurs. The reduced space creates pressure on the spinal cord or exiting nerve roots, producing a characteristic cramping, aching, or heaviness in the legs, often described as neurogenic claudication.
A hallmark feature of spinal stenosis pain is that it worsens with walking or standing and improves when sitting or leaning forward, which temporarily widens the spinal canal. Patients often report being able to walk only short distances before the symptoms force them to stop and rest.
Disc Disease and Annular Tears: A Leading Cause of Chronic Back Pain
Among the structural causes of chronic back pain, intervertebral disc disease is one of the most prevalent. The discs between the vertebrae function as shock absorbers and flexible spacers. Each disc consists of a tough outer layer called the annulus fibrosus and a soft, gel-like inner core called the nucleus pulposus.
When the annulus fibrosus develops a tear, a condition called an annular tear or annular fissure, the nucleus pulposus can protrude through the tear, placing direct pressure on nearby nerve roots and triggering a powerful inflammatory response. This is the physiological basis of a herniated disc. Research indicates that 95% of lumbar disc herniations occur at the L4-L5 or L5-S1 levels, which bear the greatest mechanical stress in the spine.
The inflammatory chemicals released from the nucleus pulposus can directly sensitize pain-conducting nerve fibers within the annular tear and surrounding tissues, producing discogenic pain, a deep, persistent ache in the lower back that is often worsened by prolonged sitting, forward bending, or activities that load the spine. Importantly, the degree of pain does not always correlate with the size of the herniation. Some patients with large herniations experience relatively little pain, while others with smaller tears report debilitating symptoms.
For a deeper understanding of disc-related conditions, including the differences between disc types and displacement patterns, visit our comprehensive guide: Disc Displacement: Types, Treatment, Recovery and Surgery Risks.
Diagnosing Chronic Back Pain
Accurate diagnosis is the foundation of effective treatment. Chronic back pain can originate from multiple sources simultaneously, making a thorough diagnostic evaluation essential. A comprehensive assessment typically includes:
• Medical history review, including the onset, duration, character, and location of pain
• Physical and neurological examination to assess strength, sensation, reflexes, and range of motion
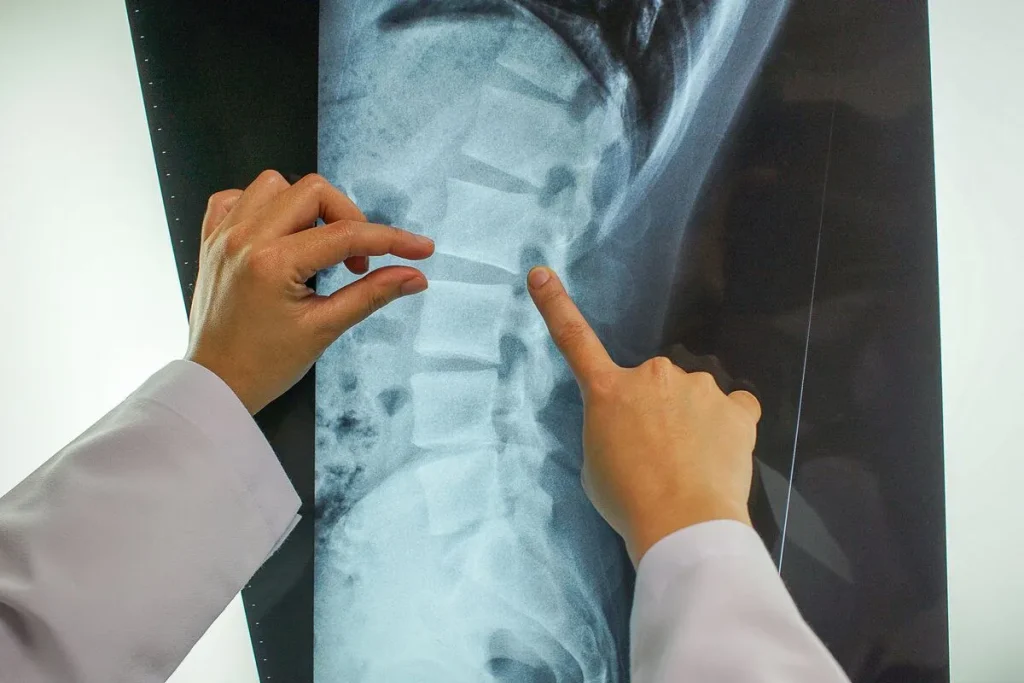
• Imaging studies, including X-ray to evaluate bone structure, MRI to assess disc health, nerve involvement, and soft tissue, and CT scan for bony detail
• Diagnostic injections, such as nerve blocks or discography, to pinpoint pain-generating structures
• Electrodiagnostic testing such as EMG or nerve conduction studies to assess nerve function
MRI is generally considered the gold standard imaging study for chronic back pain evaluation because it provides detailed visualization of disc integrity, nerve root compression, and spinal cord health. However, MRI findings must always be interpreted in the context of the patient’s clinical presentation. Studies consistently show that MRI abnormalities, including disc bulges and mild herniations, are frequently found in people with no symptoms at all, meaning that an imaging finding alone does not establish the source of pain.
Deuk Spine Institute offers the Deuk Spine Exam, a specialized evaluation that combines clinical assessment with advanced MRI interpretation to determine with high accuracy whether pain originates from a specific disc. This evaluation can be performed remotely via video consultation, making it accessible to patients across the country and internationally.
Conservative Treatment Options for Chronic Back Pain
For most patients, the initial approach to chronic back pain involves a structured trial of conservative, non-surgical treatments. These therapies aim to reduce pain, improve function, and address the physical and psychological contributors to chronic pain. Conservative treatment is most effective when it is comprehensive, individualized, and actively engaged.

Physical Therapy and Exercise
Exercise is one of the most extensively studied and consistently supported treatments for chronic low back pain. A 2025 systematic review and meta-analysis published in The Lancet Rheumatology found that exercise interventions reduced chronic low back pain intensity and disability at long-term follow-up of one to two years and beyond. 2 Additionally, a 2025 network meta-analysis published in Frontiers in Public Health examined multiple exercise prescription variables and found that sessions lasting 15 to 30 minutes produced the most significant improvements in chronic low back pain outcomes. 3
A well-designed physical therapy program for chronic back pain includes:
- Core stabilization exercises to strengthen the deep abdominal and paraspinal muscles that support the lumbar spine
- Flexibility and mobility work to reduce stiffness and restore normal movement patterns
- McKenzie Method exercises for patients with centralization of symptoms
- Postural correction and ergonomic training to minimize provocative spinal loading
- Low-impact cardiovascular conditioning, including walking, swimming, and stationary cycling
It is important to note that not all exercises are appropriate for all patients. High-impact activities, heavy loaded spinal flexion, and exercises that consistently worsen symptoms should be avoided. A spine-specialized physical therapist can design a program tailored to the specific diagnosis and severity of each patient.
Heat, Cold, and Topical Therapies
Thermal therapies remain widely used as low-cost, accessible adjuncts to back pain management. Heat therapy increases local blood flow, relaxes muscle spasm, and can provide temporary relief for muscle-related and stiffness-related pain. Cold therapy reduces acute inflammation and numbs local pain pathways, making it useful in the first 48 to 72 hours after a pain flare or minor injury.
While thermal therapies do not address underlying structural causes, they can meaningfully reduce pain intensity in the short term and enable patients to engage more effectively in therapeutic exercise.
Medications
Several classes of medication are used in the management of chronic back pain, each with distinct mechanisms, benefits, and risks:
- Nonsteroidal anti-inflammatory drugs (NSAIDs): Reduce inflammation and pain. Useful for short-term management but associated with gastrointestinal, cardiovascular, and renal risks with prolonged use.
- Muscle relaxants: Address muscle spasm and tension. Generally recommended for short-term use due to sedative side effects.
- Antidepressants (particularly SNRIs and tricyclics): Evidence supports their use in chronic pain management through effects on central pain processing, independent of their antidepressant effects.
- Topical analgesics: Creams and patches containing NSAIDs or lidocaine can reduce localized pain with minimal systemic exposure.
- Opioids: Reserved for severe, refractory cases and used with caution due to well-established risks of dependence, tolerance, and adverse effects.
A 2025 analysis of 301 clinical trials published by researchers at the University of New South Wales found that for chronic low back pain, the treatments with the best evidence of effectiveness included exercise, spinal manipulation, taping, antidepressants, and TRPV1 agonists, though all effects were described as modest.
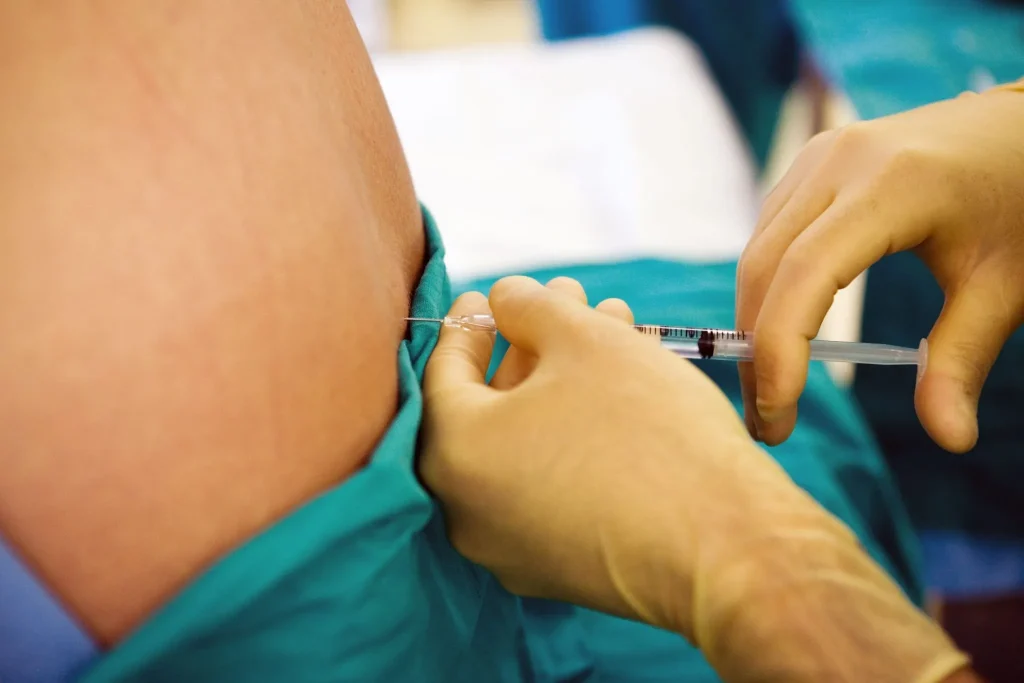
Injection-Based Therapies
Injection therapies can serve both diagnostic and therapeutic roles in chronic back pain management. Administered under fluoroscopic or ultrasound guidance, these procedures deliver medication precisely to the pain-generating structure:
Cognitive Behavioral Therapy and Mind-Body Approaches
The relationship between chronic pain and the nervous system is bidirectional. Psychological factors including catastrophizing, fear of movement, depression, anxiety, and sleep disturbance can amplify pain signals and reduce treatment effectiveness. Cognitive behavioral therapy (CBT) addresses these factors by helping patients reframe their beliefs about pain, improve coping strategies, and engage more actively in recovery-oriented behaviors.

Research consistently demonstrates that CBT improves functional outcomes, reduces pain catastrophizing, and decreases disability in chronic back pain patients. A 2024 study published in Frontiers in Pain Research investigated a novel approach called Psychophysiologic Symptom Relief Therapy (PSRT), which conceptualizes non-specific chronic back pain as having significant psychophysiologic origins and teaches patients to reinterpret pain signals as non-threatening. Early results from pilot trials showed promising reductions in pain intensity.
Mindfulness-based interventions have also demonstrated benefit. By reducing reactivity to pain sensations and improving present-moment awareness, mindfulness training can decrease pain catastrophizing and enhance quality of life. A 2024 study found that virtual therapeutic yoga programs significantly improved pain and function in patients with chronic low back pain. 4
Sleep and Lifestyle Modifications
Sleep and chronic pain have a well-established bidirectional relationship. Poor sleep amplifies pain sensitivity through multiple neurological pathways, while chronic pain disrupts the ability to fall and stay asleep. Addressing sleep hygiene, including maintaining a consistent sleep schedule, creating a comfortable sleep environment, avoiding stimulants before bedtime, and seeking treatment for sleep disorders, can meaningfully improve pain outcomes.

Additional lifestyle modifications with evidence-based support for chronic back pain include:
- Weight management: Excess body weight, particularly abdominal obesity, increases compressive load on lumbar discs and joints. Research from the Global Burden of Disease Study 2021 confirmed high BMI as one of the three most significant modifiable risk factors for low back pain.
- Smoking cessation: Smoking impairs disc nutrition, accelerates disc degeneration, and is associated with both higher rates and greater severity of chronic back pain.
- Ergonomic optimization: Proper workstation setup, monitor height, chair support, and regular movement breaks reduce cumulative spinal loading.
- Stress management: Psychological stress activates inflammatory pathways and increases muscle tension, both of which contribute to back pain.
When Conservative Treatment Is Not Enough: Advanced and Surgical Options
For most patients with chronic back pain, a structured program of conservative care lasting 8 to 12 weeks provides meaningful improvement. However, when pain persists despite comprehensive conservative treatment, when neurological deficits are progressing, or when imaging confirms a structural problem that is unlikely to resolve on its own, more advanced interventions may be appropriate.
At this stage, many patients are told that spinal fusion is their only surgical option. This is not always accurate. At Deuk Spine Institute, we offer patented minimally invasive procedures that address the root cause of pain without the collateral damage and long recovery times associated with traditional open spine surgery.
Deuk Laser Disc Repair (DLDR)
Deuk Laser Disc Repair® is the most advanced minimally invasive endoscopic spine procedure available for discogenic pain. Developed and patented by board-certified neurosurgeon Dr. Ara Deukmedjian, the procedure treats the posterior annular tear, the actual structural source of discogenic pain, through a tiny incision less than a quarter-inch in length.
Using an endoscopic camera and a Holmium YAG laser, Dr. Deukmedjian precisely removes only the painful, inflamed disc material within and around the annular tear, typically representing just 5 to 10% of the disc volume. Because the vast majority of the disc remains intact and functional, no fusion is required. The natural disc continues to provide cushioning and allows normal spinal motion.
Key features and outcomes of Deuk Laser Disc Repair® include:
- Performed through a less-than-quarter-inch incision under sedation, with no general anesthesia required
- Zero bone removal, preserving full structural integrity of the spine
- Surrounding muscles, nerves, and blood vessels remain undisturbed
- Patients typically ambulate within hours and return to normal activities within days
- 99.6% patient-reported success rate in eliminating disc-related pain across over 2,700 patients treated
- No major or minor complications reported
- No need for fusion, hardware, or implants
Unlike traditional discectomy or fusion surgery, DLDR preserves natural spinal mechanics and does not accelerate degeneration at adjacent vertebral levels, a common complication of fusion procedures.
Deuk Plasma Rhizotomy
For patients whose chronic back pain originates primarily from facet joint arthritis, Deuk Plasma Rhizotomy® offers a revolutionary minimally invasive solution. Using a patented technique involving a 4-millimeter incision, the pain-conducting nerves to the arthritic facet joint are precisely targeted and permanently disconnected, providing long-term relief without fusion or hardware.
Many patients with multilevel degenerative disc disease experience pain from both disc pathology and concurrent facet joint arthritis. In these cases, both procedures can be performed to address the full spectrum of pain sources. Learn more about managing complex, multilevel spinal conditions in our comprehensive guide on multilevel degenerative disc disease.
The Deuk Spine Exam: A Free Remote Consultation
One of the barriers to appropriate spine care is geographic. Many patients in pain are not sure whether they are candidates for advanced procedures, or they assume that traveling to a specialist is out of reach. Deuk Spine Institute offers a free remote MRI review and consultation through the Deuk Spine Exam, which can determine with 99% accuracy whether a patient’s pain originates from a disc and whether they are a candidate for Deuk Laser Disc Repair®.
End your back pain with minimally invasive spine surgery at Deuk Spine Institute. Book your free consultation today.

The Role of the Brain in Chronic Back Pain
Emerging research has increasingly recognized the role of the brain and central nervous system in perpetuating chronic back pain. A study from the University of Colorado Anschutz Medical Campus found that when patients were helped to understand that their pain involved brain processes rather than solely structural damage, they achieved better outcomes. The researchers noted that pain can function as a ‘false alarm’ generated by the nervous system, and that reframing this understanding can reduce pain intensity. 5
This does not mean chronic back pain is imaginary or purely psychological. Structural pathology, when present, must be addressed. However, incorporating pain neuroscience education, psychological support, and mind-body approaches alongside structural treatment produces the best outcomes for the largest number of patients.
Prevention: Reducing the Risk of Chronic Back Pain
While not all chronic back pain is preventable, many of the risk factors that contribute to its development and progression are modifiable. The following strategies have the strongest evidence base for protecting long-term spinal health:
- Regular, structured exercise with emphasis on core strength, spinal mobility, and cardiovascular fitness
- Maintaining a healthy body weight to reduce compressive load on lumbar discs and joints
- Avoiding tobacco products, which impair disc nutrition and accelerate degeneration
- Using proper biomechanics during lifting: engage the core, bend at the hips and knees, keep the load close to the body, and avoid twisting while lifting
- Optimizing workstation ergonomics for individuals who spend long hours sitting
- Taking regular breaks from prolonged static postures, whether seated or standing
- Addressing psychological stress, anxiety, and sleep disturbance early, as these are established risk factors for the transition from acute to chronic pain
- Seeking appropriate medical evaluation early rather than waiting for pain to become entrenched
When to See a Spine Specialist
Many people attempt to manage chronic back pain on their own, often cycling through treatments that address symptoms without reaching the root cause. Seeing a specialist becomes critical in the following situations:
- Back pain that has persisted for 12 weeks or longer without adequate improvement
- Pain accompanied by numbness, tingling, or weakness in the legs or feet
- Pain that significantly interferes with work, sleep, or daily activities
- Loss of bladder or bowel control, which is a medical emergency requiring immediate evaluation
- Progressive neurological symptoms
- Back pain following trauma such as a fall, car accident, or sports injury
- Pain that worsens despite conservative treatment
At Deuk Spine Institute, our team specializes in identifying the precise source of chronic back pain and matching each patient to the treatment most likely to produce lasting relief. Whether you have been living with pain for months or years, a definitive diagnosis and the right treatment plan can change the trajectory of your condition.

Frequently Asked Questions
Q: How long does chronic back pain last?
A: Chronic back pain is defined as pain lasting 12 weeks or more. Without appropriate treatment, it can persist for years or even decades. However, with an accurate diagnosis and the right treatment plan, including physical therapy, pain management, and when appropriate, minimally invasive surgical intervention, many patients achieve substantial or complete pain relief.
Q: Can chronic back pain be cured, or only managed?
A: The answer depends on the underlying cause. Pain driven by structural pathology, such as a herniated disc with an annular tear, can often be cured rather than merely managed. Deuk Laser Disc Repair® has achieved a 99.6% patient-reported success rate in eliminating discogenic pain in properly selected candidates. Pain from other sources, including multi-factorial or centrally mediated chronic pain, may be significantly improved through comprehensive biopsychosocial treatment programs, even if complete cure is not always achievable.
Q: Is surgery always necessary for chronic back pain?
A: No. The majority of patients with chronic back pain improve with a structured program of conservative treatment that may include physical therapy, exercise, medications, injections, and psychological support. Surgery is considered when conservative treatment has failed after an adequate trial, when there is a clear structural cause that can be corrected, or when progressive neurological deficits are present. When surgery is appropriate, minimally invasive options like Deuk Laser Disc Repair offer superior outcomes and dramatically faster recovery compared to traditional open surgery.
Q: What is the difference between acute and chronic back pain?
A: Acute back pain lasts less than four weeks and typically resolves on its own with rest, heat or cold therapy, and over-the-counter pain relief. Subacute back pain lasts four to twelve weeks. Chronic back pain is pain that persists beyond twelve weeks regardless of its original cause. Chronic pain is more likely to involve central sensitization, psychological contributors, and structural pathology that requires targeted treatment rather than watchful waiting.
Sources
1. GBD 2021 Low Back Pain Collaborators. Global, regional, and national burden of low back pain, 1990-2020. Lancet Rheumatology, 2023. https://pubmed.ncbi.nlm.nih.gov/37273833/
2. Jenkins H et al. Long-term effectiveness of non-surgical interventions for chronic low back pain: a systematic review and meta-analysis. The Lancet Rheumatology, 2025. https://doi.org/10.1016/S2665-9913(25)00064-5
3. Frontiers in Public Health. Exercise prescription for improving chronic low back pain in adults: a network meta-analysis, 2025. https://doi.org/10.3389/fpubh.2025.1512450
4. Cleveland Clinic. Research shows therapeutic virtual yoga program can be effective for chronic low back pain. ScienceDaily, 2024. https://www.sciencedaily.com/releases/2024/11/241101123525.htm
5. University of Colorado Anschutz Medical Campus. New study provides evidence for more effective brain-based treatment of chronic back pain. ScienceDaily/CU Anschutz News, 2023. https://news.cuanschutz.edu/news-stories/new-study-provides-evidence-for-more-effective-brain-based-treatment-of-chronic-back-pain