Your spine surgeon just recommended a laminectomy. Maybe a discectomy. Maybe both, followed by fusion. What nobody explained is that these procedures require drilling through bone, stripping muscle from your vertebrae, and permanently removing structural tissue your spine needs to stay stable. And once that bone is gone, it never grows back.
After over 30 years performing spine surgery and treating more than 250,000 patients across over 5,000 procedures, I’ve watched the consequences of unnecessary bone removal play out in thousands of patients. They come to me after a laminectomy that was supposed to fix them. Their original pain is still there because the surgery didn’t treat what was actually causing it. But now they also have new problems, instability, muscle damage, scar tissue, and a surgeon recommending fusion as the next step. Bone-sparing spine surgery through endoscopic techniques avoids this entire destructive cycle by treating the actual pain source without removing the structures your spine depends on.
What Laminectomy and Discectomy Actually Do to Your Spine
Most patients don’t fully understand what happens during a laminectomy or discectomy until after it’s been done. Let me be specific about the structural damage these procedures cause.
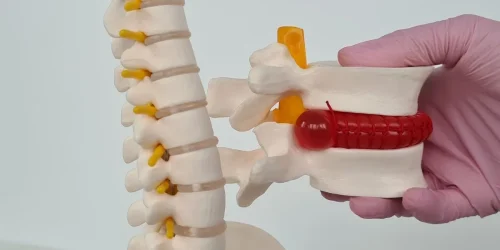
A laminectomy removes the lamina, the bony arch that protects the back of your spinal canal. The surgeon makes a 3-inch incision, strips the paraspinal muscles off the bone, then drills or cuts away the lamina along with portions of the ligamentum flavum and sometimes the facet joints. The goal is to create more space for the spinal nerves by removing bone that’s supposedly causing compression.
A discectomy removes disc material, but the traditional open approach still requires cutting through muscle and often removing bone to access the disc. Both procedures involve significant soft tissue disruption that takes months to heal, if it heals properly at all.
Here is what these procedures destroy.
- Lamina bone provides posterior structural support for your spine. Once removed, that mechanical support is permanently gone. Bone does not regenerate in this context.
- Paraspinal muscles are stripped from their bony attachments during the surgical approach. This causes denervation, atrophy, and fatty infiltration of the muscle tissue. These muscles never fully recover their original strength or function.
- Ligamentum flavum connects adjacent laminae and contributes to spinal stability during movement. Removing it eliminates a key stabilizing structure.
- Facet joint capsules and bone are frequently damaged or partially removed during a laminectomy. Facet joints bear 20 to 30% of the spine’s compressive load. Damaging them accelerates arthritis and instability.
The result is a spine that has been structurally weakened at the surgical level. This isn’t a theoretical concern. It’s a documented, predictable consequence of removing load-bearing bone and stabilizing soft tissue from a moving segment of the spine.
Why Laminectomy Leads to More Surgery
Laminectomy and discectomy are destructive to spinal stability and eventually lead to more pain. This is not my opinion. It is the biomechanical reality of removing structural tissue from a spine that still needs to support your body weight, absorb shock, and allow movement.
If a laminectomy is performed properly to treat stenosis, surgeons must remove so much bone and ligament that postoperative instability and fusion become unavoidable. Think about what that means. The “successful” version of a laminectomy, one that actually decompresses the spinal canal adequately, removes enough structural tissue to destabilize the spine. The surgeon then has to fuse the level to compensate for the damage the surgery itself created.

This is the progression that plays out in surgical suites every day.
- A laminectomy removes bone and ligament to decompress the spinal canal
- Postoperative instability develops because critical stabilizing structures are gone
- Fusion surgery is recommended to re-stabilize the spine with metal hardware
- Adjacent segment disease develops because fusion transfers mechanical stress to levels above and below
- Additional fusion is recommended to address the new degeneration at adjacent levels
Invasive procedures like a laminectomy are “entry-level” stenosis procedures that often lead to more invasive treatments like spinal fusion. Each surgery creates new problems that require the next surgery to fix. The patient enters a cycle of escalating interventions, each one more destructive than the last, each one removing more of the spine’s natural structure and replacing it with metal.
This is post-laminectomy syndrome. Failed back surgery syndrome. Whatever name you give it, the mechanism is the same. Bone removal creates instability. Instability creates pain. Pain leads to more surgery. More surgery removes more structure. The cycle continues until there is nothing left to remove, and the patient has a multi-level fusion with permanent activity restrictions.
Most Spine Surgeries Miss the Actual Pain Source
Here is the deeper problem that makes all of this worse. In most cases of chronic back pain, the laminectomy shouldn’t have been performed in the first place because it doesn’t treat what’s actually causing the pain.
Through clinical practice across thousands of patients, I’ve identified that approximately 85% of chronic back pain originates from disc injuries. Annular tears alone do not cause symptoms. The pain begins when nucleus pulposus material herniates into the tear in the posterior annulus fibrosus, triggering chronic inflammation. Over time, new pain nerve fibers grow into the inflamed tissue through a process called neoinnervation, amplifying the pain signals. The average patient has five pain generators contributing simultaneously.
Laminectomy doesn’t address annular tears. It doesn’t remove inflammatory tissue from inside a damaged disc. It doesn’t treat the actual source of pain in the vast majority of chronic back pain patients. It removes bone to create space for nerves, which may help with leg symptoms from stenosis, but does nothing for the disc-related pain that brought the patient to surgery in the first place.
Most spine surgeons were never trained to identify annular tears during residency. They learned decompression for stenosis, fracture stabilization, tumor removal, and fusion. They were not trained to identify and treat painful disc issues. Board certification alone does not indicate specialized spine expertise, high procedure volumes, or advanced training in identifying pain generators. It only indicates completion of residency and passing exams. So surgeons recommend what they know. And what they know involves drilling through bone.
There is another layer to this problem. Spinal stenosis produces leg symptoms like heaviness, cramping, and weakness with walking. It does not cause back pain. If a patient has both stenosis and back pain, those are separate conditions requiring separate treatment. Yet the laminectomy addresses only the stenosis while ignoring the disc injury generating the back pain. The patient wakes up from surgery, and their legs may feel better, but their back still hurts. Because nobody treated the annular tear.
How Endoscopic Laser Surgery Preserves Your Spine
Endoscopic spine surgery through Deuk Laser Disc Repair® takes the opposite approach. Instead of removing bone, muscle, and ligament to create a wide surgical corridor, it accesses the damaged disc through a 4mm cervical or 7mm lumbar incision using an endoscope the width of a pencil. No bone is drilled. No bone is removed. No muscle is stripped from the spine. No ligaments are cut.
The endoscope passes through natural anatomical pathways to reach the disc. Once inside, laser technology removes the inflammatory tissue from within the annular tear, extracts the herniated nucleus pulposus material causing irritation, and debrides the damaged tissue. The tear then heals naturally over 9 to 12 months without cadaver bone, metal hardware, or plastic spacers.
Every structure your spine needs for long-term stability remains intact.
- Lamina bone stays in place, maintaining posterior structural support
- Paraspinal muscles are dilated rather than stripped, preserving their attachments and function
- Ligamentum flavum remains intact, continuing to stabilize the segment
- Facet joints are completely untouched, maintaining their load-bearing function
- Disc height and motion are preserved because the disc itself is repaired, not removed
This is why bone-sparing spine surgery produces better long-term outcomes. By preserving every structural element, the treated level continues to function normally. There is no postoperative instability. No need for fusion. No adjacent segment disease from altered biomechanics. The destructive cascade that begins with a laminectomy never starts.
The Clinical Difference in Outcomes
The numbers tell the story clearly. Over 2,732 Deuk Laser Disc Repair® procedures have been performed with zero surgical complications, zero infections, zero spinal fluid leaks, zero nerve injuries, and zero emergency reoperations. Peer-reviewed publications report outcomes of 99% pain elimination when the diagnosed pain source matches the treated pathology.
Compare that to a traditional laminectomy and fusion. Industry-wide complication rates range from 5 to 50%. Infection occurs in 1 to 3% of cases. Dural tears occur in 2 to 8%. Nerve injury occurs in 1 to 2%. Reoperation within five years occurs in 10 to 15%.
The recovery comparison is equally dramatic.
- Deuk Laser Disc Repair® uses a 4mm or 7mm incision, takes approximately 20 minutes per disc, patients walk shortly after, go home the same day, need no opioid narcotics because there is minimal to no internal trauma, and return to work within 3 days with lifting restrictions
- Traditional laminectomy with fusion requires a 3-inch incision, bone removal, hardware implantation, general anesthesia, a 3 to 5 day hospital stay, mandatory opioid narcotic prescriptions with high potential for addiction and overdose, and 6 to 12 months of recovery
These are not marginal differences. One approach preserves your spine. The other permanently alters it.
Why Diagnosis Determines Everything
No surgery, regardless of technique, produces good outcomes when it treats the wrong problem. An MRI is a picture of anatomy, not a diagnosis of pain. MRIs never tell you where pain comes from. 100% of people over age 45 have disc herniations on MRI, whether they have pain or not. Only 10 to 15% are symptomatic. Radiologists miss disc bulges from annular tears more than 50% of the time.

The Deuk Spine Exam® combines focused physical examination, pain history analysis, and MRI correlation to achieve 99% diagnostic accuracy in identifying every structural pain generator. Over 10,000 evaluations have been performed, and the exam can be completed virtually over video conference in approximately 10 minutes. This matters because roughly 90% of our patients travel from other states or countries due to a lack of local surgeons with equivalent endoscopic training, volume, or published outcomes.
The exam identifies all five major pain generators, disc injuries, facet joint arthritis, sacroiliac joint dysfunction, piriformis syndrome, and compression fractures, then creates a treatment plan addressing every symptomatic structure. The exam also distinguishes true nerve compression from nerve irritation secondary to disc inflammation. Many patients recommended for a laminectomy have leg pain from nerve irritation, not compression. Laminectomy cannot help those patients because there is nothing to decompress. When the annular tear is treated instead, the inflammation resolves and the leg pain disappears without any bone removal. For facet joint pain, the Deuk Plasma Rhizotomy® permanently destroys pain-mediating nerves inside the joint. For piriformis syndrome, the Deuk Piriformis Release® addresses chronic scar tissue through a 4mm incision. Multiple pain generators can be treated in the same session.
Your Spine Doesn't Need to Be Destroyed to Be Fixed
If you’ve been recommended for a laminectomy, discectomy, or fusion, you owe it to yourself to understand what those procedures will permanently remove from your spine and whether a bone-sparing approach can treat the same condition while preserving everything your spine needs for long-term stability.
Deuk Spine Institute offers a free MRI review to evaluate whether your condition is treatable with endoscopic, bone-sparing techniques. Over 3,000 reviews have been completed. After over 30 years of performing spine surgery, completing 2,500+ cervical and 3,000+ lumbar procedures, I can tell you that the vast majority of patients recommended for a laminectomy or fusion have a disc injury that can be treated without removing a single piece of bone.
Request your free MRI review today. Find out if your spine can be treated without being destroyed.