Herniated disc symptoms vary dramatically depending on where in your spine the herniation occurs – and whether it is pressing on a nerve. Some people walk around with a herniated disc on MRI and feel nothing. Others can barely get out of bed. The difference almost always comes down to nerve compression.
At Deuk Spine Institute, Dr. Ara Deukmedjian has performed over 2,000 minimally invasive spine procedures and built a diagnostic methodology with 99% accuracy in identifying the true pain source. In this guide, we break down every major herniated disc symptom by spinal location, explain when symptoms indicate a medical emergency, and show you what diagnosis actually looks like from an expert neurosurgeon’s perspective.
What Causes Herniated Disc Symptoms?
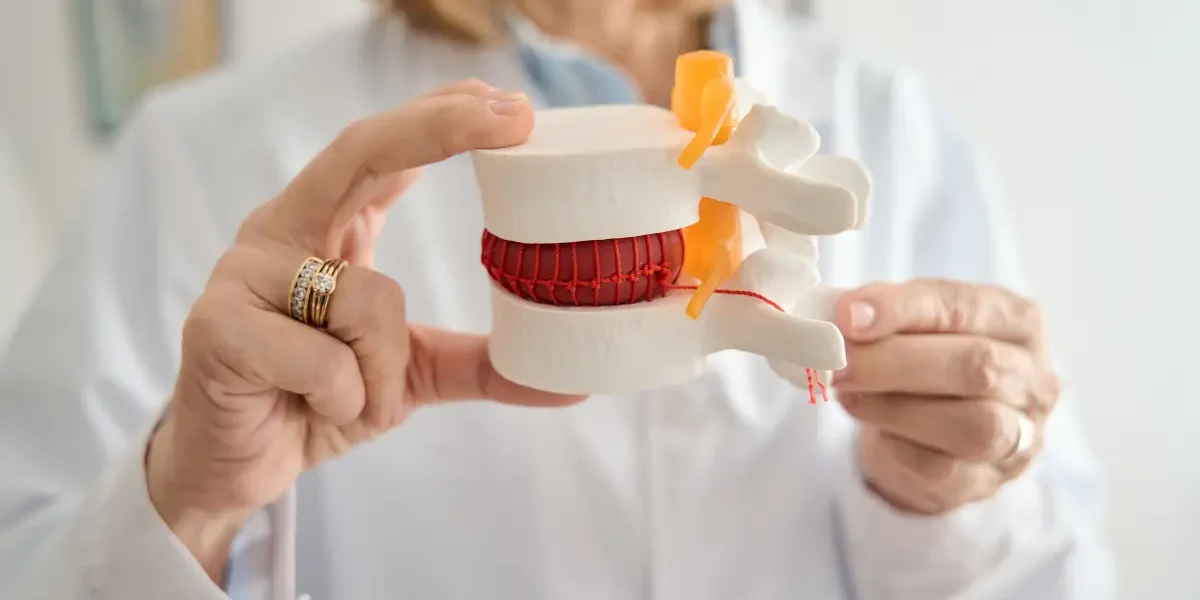
A disc herniation occurs when the soft, gel-like inner material of an intervertebral disc – called the nucleus pulposus – pushes through a tear in the tough outer ring, known as the annulus fibrosus. When that displaced material contacts a nearby nerve root, it triggers two things simultaneously: mechanical pressure on the nerve and a chemical inflammatory response.
Both mechanisms cause symptoms. The mechanical compression produces the sharp, electric-shock radiating pain most people associate with a pinched nerve. The chemical inflammation causes swelling around the nerve root, which can sustain pain even after the physical pressure is reduced.
This is why herniated disc symptoms rarely resolve completely with anti-inflammatories alone – you can reduce the inflammation response, but the structural problem driving it remains.
Herniated Disc Symptoms by Location
The spine is divided into three regions: cervical (neck), thoracic (mid-back), and lumbar (lower back). Each produces a distinct symptom pattern when a disc herniates, because each region houses different nerve roots that control different body areas.
Cervical Herniated Disc Symptoms (Neck)
The cervical spine spans C1 through C7 at the base of your neck. Herniations here most commonly occur at C5-C6 and C6-C7, where the neck handles the greatest degree of motion and mechanical stress. Cervical disc herniation symptoms include:
- Neck pain – ranging from a deep ache to sharp pain that worsens with specific head positions
- Arm pain (cervical radiculopathy) – burning, shooting, or electric sensations traveling down one arm; the specific path depends on which nerve root is compressed
- Numbness and tingling – often felt in the fingers or forearm; commonly mistaken for carpal tunnel syndrome
- Shoulder blade pain – a dull, persistent ache near or between the shoulder blades
- Grip weakness – difficulty holding objects, opening jars, or maintaining hand strength
- Biceps or triceps weakness – depending on whether C5-C6 or C6-C7 is involved
A herniation at C5-C6 typically affects the C6 nerve root, producing pain and sensory changes running down the outside of the forearm into the thumb and index finger, along with weakness in the biceps and wrist extensors.
A herniation at C6-C7 – the most common site of cervical radiculopathy – compresses the C7 nerve root. Symptoms follow the back of the arm into the middle finger, with triceps weakness and a diminished triceps reflex.
Thoracic Herniated Disc Symptoms (Mid-Back)
Thoracic disc herniations are less common because the rib cage provides structural stability to the mid-spine. When they occur, they produce a distinctive and often confusing symptom pattern:
- Mid-back pain – localized aching between the shoulder blades or along the ribs
- Band-like chest or abdominal pain – a wrapping, constricting sensation that follows the path of the compressed thoracic nerve around the torso; frequently misdiagnosed as cardiac or digestive problems
- Intercostal neuralgia – sharp, stabbing pain along a specific rib line
- Lower extremity symptoms – if the herniation is large enough to compress the spinal cord rather than a nerve root, symptoms can include leg weakness, balance problems, or difficulty walking
Because the thoracic spinal canal is narrower than the lumbar canal, even a moderate herniation here can cause myelopathy – spinal cord compression – which produces neurological symptoms well below the level of injury.
Lumbar Herniated Disc Symptoms (Lower Back)
The lumbar spine is where the majority of disc herniations occur. L4-L5 and L5-S1 bear the greatest mechanical load and are the most frequent sites. Lumbar herniated disc symptoms include:
- Lower back pain – may be localized, diffuse, or worsened by bending, twisting, and prolonged sitting
- Sciatica – the hallmark symptom of lumbar disc herniation; a sharp, burning, or electric pain that radiates from the lower back through the buttock and down the leg; the specific path identifies which nerve root is compressed
- Leg numbness or tingling – follows the same nerve root distribution as the pain, often into the foot or toes
- Muscle weakness – difficulty walking on tiptoes (L5-S1 involvement) or heel-walking (L4-L5 involvement)
- Pain that worsens with sitting – sustained disc compression in a seated position amplifies nerve irritation
- Morning stiffness – discs rehydrate overnight, increasing in height by up to 20%; when a herniation is present, this overnight swelling can temporarily worsen nerve compression first thing in the morning
At L4-L5, herniation typically compresses the L5 nerve root. Pain and sensory changes travel down the outer thigh and leg to the top of the foot and between the first and second toes. Foot drop – difficulty lifting the front part of the foot – can develop with significant nerve compromise.
At L5-S1, herniation affects the S1 nerve root. Pain travels down the back of the thigh and calf to the heel and outer edge of the foot. Weakness when standing on tiptoes is a characteristic finding.
Herniated Disc Symptoms by Severity
Not all herniated discs produce the same intensity of symptoms. The degree of nerve compression, the presence of inflammation, and the individual patient’s anatomy all influence how severe symptoms become.
Mild Symptoms
Early or mild herniation may produce only localized back or neck pain without significant nerve involvement. Patients may notice:
- Intermittent aching that comes and goes
- Stiffness after sleeping or prolonged sitting
- Pain with specific movements (bending, reaching, rotating)
- Occasional mild tingling that resolves quickly
Mild symptoms do not necessarily mean a mild structural problem. Many patients have significant herniation on MRI with minimal symptoms – until the disc material shifts further and acute nerve compression develops.
Moderate Symptoms
As nerve compression increases, symptoms become more consistent and disruptive:
- Persistent radiating pain into an arm or leg
- Numbness or tingling that does not fully resolve
- Difficulty with specific activities (lifting, bending, walking distances)
- Sleep disruption from positional pain
- Reduced grip strength or leg stability
Moderate symptoms typically signal that the herniated disc material is in consistent contact with a nerve root. Conservative treatment may reduce inflammation temporarily, but the underlying disc damage is not self-correcting at this stage.
Severe Symptoms
Severe nerve compression produces symptoms that significantly impair daily function:
- Constant, debilitating radiating pain unresponsive to position changes
- Progressive muscle weakness that limits walking or arm use
- Near-complete numbness in the affected limb
- Loss of reflexes (absent biceps, triceps, or Achilles reflex)
Severe symptoms require prompt evaluation. Prolonged, untreated nerve compression can lead to permanent nerve damage even after the structural problem is corrected.
Emergency Warning Signs: When to Go to the ER
Most herniated disc symptoms, while painful, are not life-threatening emergencies. But several warning signs require immediate emergency evaluation – not a scheduled appointment, not a call to your primary care doctor. The ER. Today.
These are the red flag symptoms of cauda equina syndrome – a surgical emergency caused by compression of multiple nerve roots in the lower lumbar spine:
- Sudden loss of bladder control – inability to urinate or involuntary urination you cannot control
- Sudden loss of bowel control – incontinence or inability to feel the need to have a bowel movement
- Saddle anesthesia – numbness in the inner thighs, groin, buttocks, or genital area (the region that would contact a saddle)
- Rapidly progressive leg weakness – weakness developing over hours that is getting worse, not stable
- Sexual dysfunction with sudden onset – loss of sensation or function not previously present
Waiting even 24 to 48 hours with cauda equina symptoms can result in permanent paralysis, permanent incontinence, and irreversible nerve damage. This is not a situation where a wait-and-see approach is acceptable.
Symptoms That Are Often Mistaken for a Herniated Disc
One of the most important clinical distinctions in spine care is recognizing what is – and what is not – caused by a herniated disc. Several conditions produce overlapping symptoms that lead to years of misdiagnosis and ineffective treatment.
Piriformis Syndrome
The piriformis muscle runs directly over the sciatic nerve in the buttock. When it tightens or spasms, it can compress the sciatic nerve and produce sciatica-like symptoms almost identical to L5-S1 disc herniation. Patients with piriformis syndrome often have normal lumbar MRI findings despite significant leg pain. The distinction requires clinical examination by a specialist who understands both conditions.
Facet Joint Disease
Facet joints connect each vertebra in the spine. When these joints degenerate, they can produce localized back or neck pain, sometimes with referred pain into the shoulder or buttock region. Unlike disc herniation, facet joint pain rarely travels below the knee and is not associated with true radicular arm or leg symptoms. Patients are frequently told they have a herniated disc when the actual pain source is the facet joint – and vice versa.
Carpal Tunnel Syndrome
C6 and C7 nerve root compression from a cervical herniation produces numbness and tingling in the fingers – exactly the symptoms carpal tunnel syndrome causes. The differentiation requires nerve conduction studies and a careful evaluation of where symptoms originate. Treating carpal tunnel when the actual problem is a cervical disc herniation provides no lasting relief.
Spinal Stenosis
Stenosis is a narrowing of the spinal canal that compresses the spinal cord or nerve roots. It can mimic disc herniation symptoms closely. The critical distinction is that stenosis typically worsens with standing and walking (neurogenic claudication) and improves with sitting or bending forward – the opposite pattern from most disc herniations.
How Herniated Disc Symptoms Are Diagnosed
Accurate diagnosis is the foundation of effective treatment. At Deuk Spine Institute, Dr. Deukmedjian uses the Deuk Spine Examination – a proprietary diagnostic methodology with 99% accuracy – that correlates MRI findings directly with clinical symptoms to identify the true pain source.
MRI: The Gold Standard
MRI is the most accurate imaging tool for diagnosing disc herniation. It provides detailed visualization of the disc itself, the extent of herniation, the degree of nerve root compression, and associated soft tissue changes. A critical point that most patients do not realize: MRI findings alone do not determine treatment.
Research shows that disc abnormalities are present in up to 60% of asymptomatic individuals over age 50. A disc that appears herniated on MRI may or may not be the actual source of a patient’s pain. Accurate diagnosis requires correlating the MRI with a thorough clinical examination and a precise account of symptom location, character, and behavior.
Physical Examination
An experienced neurosurgeon uses specific examination maneuvers to identify which nerve root is involved and whether symptoms match the imaging findings:
- Straight leg raise test – lifting the leg while lying flat; pain radiating below the knee at less than 60 degrees is highly suggestive of lumbar nerve root compression
- Spurling’s test – a cervical compression maneuver that reproduces radicular arm symptoms when positive; specific to cervical nerve root involvement
- Reflex testing – diminished or absent reflexes (biceps, triceps, patellar, Achilles) identify which nerve root is compromised
- Dermatomal sensory testing – mapping numbness distribution against known nerve root patterns to confirm the level of compression
CT Scan and X-Ray
X-rays show bone structures but cannot visualize discs or nerve compression directly. They may reveal indirect signs like reduced disc height or bone spurs. CT scans offer more detail than X-rays, particularly for bony anatomy, but remain less accurate than MRI for soft tissue disc assessment. CT myelography – injecting contrast dye into the spinal fluid before a CT scan – provides detailed nerve root imaging for patients who cannot undergo MRI.
Why Conventional Treatments Often Fail Herniated Disc Symptoms
The majority of patients who come to Deuk Spine Institute have already been through months – sometimes years – of conservative treatment. They have done physical therapy. They have received epidural steroid injections. They have taken muscle relaxers, NSAIDs, and in some cases opioids. And they are still in pain.
This is not a failure of effort. It is a failure of mechanism.
Conservative care addresses the inflammatory component of herniated disc pain effectively in the short term. Physical therapy can strengthen supporting musculature and improve posture mechanics. But none of these approaches correct the structural disc problem – the displaced nucleus pulposus material that is physically pressing on a nerve root does not disappear because inflammation is reduced.
Epidural steroid injections work by flooding the area around the nerve with corticosteroid. For many patients, this provides weeks to months of relief. But once the steroid effect wears off, the herniation is still there. The nerve is still being compressed. The pain returns – often to the same level or worse.
Research confirms that patients who pursue only conservative treatment for 9 to 12 months without improvement show worse surgical outcomes than those who escalate care sooner. The window for optimal treatment is not indefinite.
Herniated Disc Treatment: Beyond Conservative Care
When conservative treatment has failed – typically defined as 6 to 12 weeks of appropriate care without meaningful improvement – the structural cause of the herniation needs to be addressed directly.
Traditional spinal fusion removes the disc and fuses the two adjacent vertebrae together with bone graft and hardware. This permanently eliminates motion at the treated level and carries a risk of adjacent segment disease – accelerated degeneration of the vertebrae immediately above and below the fusion site – as those levels compensate for lost mobility.
Deuk Laser Disc Repair (DLDR) is a patented, minimally invasive endoscopic procedure developed and performed exclusively by Dr. Ara Deukmedjian. Through a quarter-inch incision, Dr. Deukmedjian uses a laser to vaporize the herniated disc material compressing the nerve root – without removing bone, without hardware implantation, and without fusing the spine. Approximately 85 to 90% of the disc remains intact. Natural disc height and spinal motion are fully preserved.
The procedure is outpatient. Patients walk out of the surgery center within one to two hours. Most return to desk work within a week and physical work within four to six weeks.
In published peer-reviewed research covering over 1,300 patients, Deuk Laser Disc Repair has achieved a 95% success rate in pain elimination with zero major complications documented in the surgical record. This is not a marketing claim – it is independently verifiable through PubMed.
For patients considering this option, learn more about how Deuk Laser Disc Repair works and what makes it fundamentally different from standard discectomy or fusion.
When to See a Spine Specialist for Herniated Disc Symptoms
Many patients wait far too long before seeking an expert evaluation. The typical timeline – primary care referral, physical therapy, pain management, injections, and finally a spine surgeon – can take two years or longer. By that point, some patients have sustained avoidable nerve damage, and others have been recommended for fusion that a more conservative minimally invasive approach could have avoided.
See a spine specialist promptly if you experience any of the following:
- Radiating arm or leg pain that does not improve within two to four weeks of rest and over-the-counter care
- Progressive numbness or weakness in an arm or leg
- Symptoms that significantly disrupt sleep, work, or daily activities
- Pain that initially improved with conservative care but has returned
- Any of the emergency symptoms listed above
If you have already seen one or more spine surgeons and been told your only option is fusion, a second opinion with a specialist who performs motion-preserving procedures is worth pursuing. Many patients recommended for fusion are appropriate candidates for less invasive alternatives.
The comprehensive herniated disc guide covers how different types of herniations – bulge, protrusion, extrusion, sequestration – compare in severity and treatment implications. For patients with neck-specific symptoms, the cervical disc herniation guide goes deeper into C-level specifics.
The Free MRI Review: Know Your Options Before You Decide Anything
Before committing to any treatment – before agreeing to injections, fusion surgery, or continued conservative care – you have the right to know what is actually causing your symptoms.
Deuk Spine Institute offers a Free MRI Review with no obligation. Dr. Deukmedjian or a member of the clinical team reviews your existing MRI, correlates the findings with your symptom history, and provides an honest assessment of whether surgical intervention is warranted, what the best option is if so, and whether your case is appropriate for Deuk Laser Disc Repair.
This review does not require a trip to Florida. It is conducted virtually – you submit your MRI and symptom history, and the review is completed remotely. Patients from across the United States and internationally use this process to get a definitive expert evaluation before making any decisions about their spine care.
If you have been living with herniated disc symptoms and have not yet had an expert neurosurgeon review your MRI, this is the lowest-friction next step available to you.
Frequently Asked Questions: Herniated Disc Symptoms
Can a herniated disc cause symptoms without lower back pain?
Yes. When a herniated disc compresses a nerve root, the radiating arm or leg pain (radiculopathy) is often the dominant or even the only symptom. Many patients with significant disc herniation have minimal axial back or neck pain and are surprised to learn the source of their arm or leg symptoms is a spinal disc. This is particularly common with cervical herniations, where finger numbness and arm pain appear with little or no neck pain.
How do I know if my sciatica is from a herniated disc or something else?
Sciatica from a herniated disc typically follows a specific dermatomal pattern – the pain and numbness travel along the path of a specific nerve root from the lower back through the buttock and down the leg to a predictable endpoint in the foot. This pattern is reproducible with certain positions and maneuvers like the straight leg raise. Sciatica from piriformis syndrome is more diffuse, rarely travels below the knee in a nerve-specific pattern, and is worsened by direct pressure over the piriformis in the buttock. An MRI and clinical examination together can distinguish between these causes with high accuracy.
Why do herniated disc symptoms feel worse in the morning?
Intervertebral discs are largely avascular – they absorb nutrients and fluid through a process called imbibition rather than a direct blood supply. During sleep, discs rehydrate and can increase in height by up to 20%. When a herniation is present, this overnight fluid gain temporarily increases the volume of the disc material pressing against the nerve root. This is why many patients experience their worst symptoms shortly after waking, before movement and gravity begin to compress the disc back down through the day.
Can herniated disc symptoms go away without surgery?
Some cases of disc herniation improve on their own, particularly smaller protrusions in younger patients where the herniated material can reabsorb over time through immune-mediated processes. Research published in 2025 has helped clarify the biological mechanisms behind spontaneous herniation reabsorption, identifying macrophage activity as a key factor. However, complete annular tear healing is rare without targeted intervention.
More commonly, symptoms may reduce as inflammation subsides while the underlying structural damage persists – meaning symptoms can return with future activity or minor reinjury. For patients with persistent or worsening symptoms beyond six weeks, continuing to wait rarely produces better outcomes.
Is herniated disc pain constant or does it come and go?
Early herniated disc pain is often positional and intermittent – aggravated by specific movements and relieved by others. As the herniation progresses or inflammatory response intensifies, pain can become more constant.
Most patients find a position of relative comfort (often lying down with knees slightly bent for lumbar herniations) but cannot maintain pain-free status throughout a full active day. The pattern of symptoms is itself diagnostically useful – a neurologist or neurosurgeon will ask specific questions about what makes symptoms better or worse to help identify the pain source.
What is the difference between a herniated disc, a bulging disc, and a ruptured disc?
These terms describe different stages or types of disc pathology:
- A bulging disc means the entire disc circumference extends slightly beyond the vertebral margins – the outer ring (annulus fibrosus) is intact but compressed.
- A herniated disc (also called a protruded or prolapsed disc) means the inner nucleus pulposus has pushed through a focal weakness or tear in the annulus.
- A ruptured disc or extruded disc means the herniated material has broken through the outer annulus entirely.
- A sequestered disc is a severe form where a fragment of disc material has broken off and is floating free in the spinal canal.
Symptoms generally worsen with advancing severity, though the correlation is imperfect – some extruded herniations cause less pain than moderate protrusions if the fragment has migrated away from the nerve.
Do I need to have leg or arm symptoms to have a herniated disc?
No. Not every herniated disc compresses a nerve root. Herniations can produce significant axial pain – localized back or neck pain – through direct irritation of pain-sensitive structures in and around the disc itself, including the annular fibers, the posterior longitudinal ligament, and adjacent structures. This is called discogenic pain. It can be severe and debilitating without producing any radiating extremity symptoms.
Accurate diagnosis of discogenic pain without radiculopathy requires experienced clinical correlation of MRI findings with the precise symptom pattern.
Can herniated disc symptoms be permanent?
When nerve compression is prolonged and severe, some degree of permanent nerve damage is possible – including persistent numbness, weakness, or reflex loss even after the structural problem is corrected. This is one of the strongest arguments for not waiting indefinitely before seeking definitive treatment.
However, many patients with what they believe is permanent numbness or weakness experience significant or complete recovery after the herniated disc material is removed and nerve decompression is achieved. The earlier the intervention, the greater the recovery potential.