By Dr. Ara Deukmedjian, MD
Board-Certified Neurosurgeon, Deuk Spine Institute
Medically reviewed on March 4, 2026
Medical Disclaimer: This content is for educational purposes only and does not constitute medical advice. Individual results may vary. Always consult with your healthcare provider about your specific condition and treatment options.
Key Points
- Cervical radiculopathy, the clinical term for a pinched nerve in the neck, develops when a nerve root in the cervical spine is compressed or chemically inflamed, producing pain, numbness, tingling, and weakness that can radiate into the arm, shoulder, and hand
- The most common causes are herniated intervertebral discs and degenerative bone spurs (osteophytes) narrowing the foramen through which nerve roots exit the spine
- Symptoms vary depending on which cervical nerve root is affected, and they can range from sharp burning pain to subtle hand weakness or loss of dexterity
- A 2025 updated review in StatPearls confirms that neck pain accounts for up to 40% of work absenteeism and that cervical radiculopathy significantly reduces function and quality of life
- A 2024 prospective multicenter study published in Scientific Reports found that arm pain was reduced the most following surgical decompression, with a mean reduction of 3.4 points on the numerical rating scale across all cervical levels
- Most patients improve with conservative care including physical therapy, cervical traction, and targeted medications, but patients with significant neurological deficits or progressive symptoms may require surgical intervention
- For eligible patients, Deuk Spine Institute offers Deuk Laser Disc Repair®, a minimally invasive outpatient procedure that removes the damaged disc material without hardware, fusion, or an overnight hospital stay
What Is a Pinched Nerve in the Neck?
You wake up with a sharp, burning sensation running from your neck down into your arm. Your fingers tingle. Turning your head to back out of the driveway feels almost impossible. These are not signs of ordinary muscle soreness. They are the hallmarks of a pinched nerve in the neck, a condition that affects millions of people and can significantly interfere with daily life if left untreated.
The medical term for a pinched nerve in the neck is cervical radiculopathy. It occurs when one of the nerve roots that branches off your spinal cord in the cervical region (the upper seven vertebrae of the spine) becomes compressed, irritated, or chemically inflamed. Once that nerve root is compromised, it cannot reliably transmit signals related to sensation and movement. The result is a distinctive pattern of symptoms that follow the path of that specific nerve root, a pattern known as a dermatome or myotome distribution.
The cervical spine contains seven vertebrae, labeled C1 through C7, separated by intervertebral discs that absorb shock and allow movement. Between each pair of vertebrae, nerve roots exit through small bony openings called foramina. When the structures surrounding these openings change due to disc herniation, bone spur formation, or injury, the nerve root inside can become squeezed.
Understanding what is happening inside your spine is the first step toward getting the right diagnosis and appropriate treatment. This guide covers everything you need to know about the symptoms, causes, diagnosis, and treatment options for a pinched nerve in the neck.
How Common Is a Pinched Nerve in the Neck?
Cervical radiculopathy is more common than many people realize. A 2025 updated review in StatPearls noted that up to 40% of work absenteeism is attributed to individuals with a history of neck pain, and that cervical radiculopathy significantly reduces both function and quality of life. 1 The condition affects people across a wide age range but tends to peak between the fourth and sixth decades of life, when degenerative disc changes and osteophyte formation are most prevalent.
The cervical nerve roots most commonly affected are C6 and C7, which correspond to symptoms felt in the forearm, hand, and fingers. However, any level from C4 through C8 can be involved, and each produces a slightly different pattern of pain, numbness, and weakness.
Pinched Nerve in the Neck: The Full Range of Symptoms
The symptoms of cervical radiculopathy can vary considerably depending on the location and severity of the nerve root compression. Some people experience intense pain from the start. Others notice subtle changes in sensation or strength that gradually worsen over weeks or months. Below is a thorough review of the symptoms you may experience.
Burning Pain in the Neck, Arm, or Shoulder
One of the most characteristic symptoms of a pinched nerve in the neck is a burning or electric pain that begins in the neck and radiates outward. This pain follows the path of the compressed nerve root, which is why it often travels down the shoulder, through the arm, and into specific fingers rather than spreading diffusely.
The burning sensation occurs because the inflamed or compressed nerve is misfiring, sending abnormal pain signals to the brain. This pain may be constant, or it may flare up with certain positions or activities. Many patients describe it as a hot, searing sensation that seems to travel like an electric current from the base of the neck down to the fingertips.

Tingling and Numbness
Tingling or numbness in the arm or hand is another hallmark symptom. Known clinically as paresthesia, this sensation is often described as pins and needles, a prickling feeling, or a sense that a part of the arm or hand has "fallen asleep" without any obvious cause.
The specific location of the tingling depends on which nerve root is involved. For example, compression of the C6 nerve root typically produces tingling in the thumb and index finger, while C7 involvement tends to cause numbness in the middle finger. C8 nerve root compression often produces tingling along the little finger and the inner edge of the hand. A 2025 scoping review published in BMC Musculoskeletal Disorders confirmed that somatosensory changes are a core component of cervical radiculopathy presentation, though they can vary widely between patients. 2

Arm or Hand Weakness
Muscle weakness in the arm, forearm, or hand is one of the more concerning symptoms of cervical radiculopathy, because it indicates that the motor component of the nerve root is being affected. Each cervical nerve root contributes to the function of specific muscle groups, so weakness tends to be localized and pattern-specific.
A patient with C5 nerve root compression may have difficulty raising the arm above the shoulder or notice weakness when bending the elbow. A patient with C7 involvement may struggle to extend the elbow or wrist. C6 compression can produce weakness in wrist extension, while C8 involvement may impair grip strength and fine motor tasks such as buttoning a shirt or holding a pen.
Muscle weakness should not be ignored or attributed to overuse or fatigue. When weakness develops alongside pain or numbness, it signals that the nerve is under enough pressure to disrupt motor signals, and this warrants prompt evaluation. Delayed treatment can allow weakness to become persistent or, in severe cases, permanent.
Pain That Radiates Down the Arm
Radiating arm pain, sometimes called brachialgia, is one of the defining features that separates cervical radiculopathy from ordinary neck muscle strain. The pain travels along the dermatome, the specific region of skin and tissue served by the affected nerve root, and is often described as sharp, shooting, or burning.
The distribution of radiating pain provides important diagnostic clues. Pain radiating into the lateral arm and thumb suggests C6 involvement. Pain radiating into the middle finger and triceps area suggests C7. Pain that runs along the inner arm and into the ring and little fingers points toward C8. This pattern-based symptom map is one of the reasons a careful clinical history remains so valuable in diagnosing this condition.
Worsening Pain at Night or at Rest
Many patients with a pinched nerve in the neck notice that pain intensifies at night or when lying down. This is counterintuitive because rest is usually associated with relief. However, lying still can allow inflammatory fluids to accumulate around the compressed nerve root, increasing pressure and pain. Certain sleeping positions can also place the cervical spine in a position that narrows the foramen further, compressing the nerve even more.
If nighttime pain is disrupting your sleep consistently, this is a signal that the nerve compression is significant and that the condition may be progressing rather than resolving on its own.

Pain That Worsens with Neck Movement
Cervical nerve root compression is almost always position-dependent. Movements that reduce the diameter of the foramen, such as tilting the head back and toward the side of symptoms (a clinical test called the Spurling maneuver), will typically provoke or intensify radicular pain. Conversely, movements that increase the foraminal space, such as lifting the arm above the head on the affected side, may provide temporary relief.
Pain that reliably worsens when looking up, rotating the head, or extending the neck is a clinically significant finding. It suggests that the nerve root is mechanically compressed by a structure that shifts with movement, such as a herniated disc or a hypertrophic facet joint.
Loss of Deep Tendon Reflexes
Reduced or absent reflexes in the arm are a neurological sign of cervical radiculopathy that a physician will check during a physical examination. The biceps reflex corresponds to C5-C6, the brachioradialis reflex to C6, and the triceps reflex to C7. A diminished or absent reflex at a specific level provides objective evidence of nerve root dysfunction at that level. A 2025 scoping review found that reduced tendon reflexes were among the most specific clinical signs for confirming cervical radiculopathy.
Neck Stiffness and Tenderness
In addition to the radiating symptoms, most patients also experience localized pain and stiffness in the neck itself. Tenderness to palpation along the posterior cervical muscles, reduced range of motion in all directions, and muscle guarding are common findings. The neck pain may be deep and aching or sharp with movement.
What Causes a Pinched Nerve in the Neck?
Several underlying conditions can lead to nerve root compression in the cervical spine. Understanding the cause is essential for selecting the most appropriate treatment.
Herniated Cervical Disc
A herniated disc is one of the most common causes of acute cervical radiculopathy, particularly in younger and middle-aged adults. The intervertebral disc is composed of a tough outer ring called the annulus fibrosus and a gel-like inner core called the nucleus pulposus. When the annulus develops a tear or crack, the nucleus can bulge outward or rupture into the spinal canal, directly compressing a nearby nerve root.
The compression from a herniated disc can be both mechanical, from the disc material physically pressing on the nerve, and chemical, from the inflammatory proteins within the nucleus pulposus that irritate the nerve tissue even without direct contact. This is why some patients with relatively small herniations experience intense pain, while others with large herniations may have minimal symptoms.
Degenerative Disc Disease and Bone Spurs
As people age, the intervertebral discs naturally lose hydration and height. This degenerative process can cause the vertebrae to move closer together, reducing the space available for nerve roots within the foramen. In response to this instability, the body may form osteophytes, or bone spurs, around the joints and disc margins. When these spurs grow into the foramen, they can compress the nerve root in a more chronic, gradual manner.
Unlike the sharp onset often seen with disc herniations, radiculopathy from degenerative changes and bone spurs tends to develop over months or years and is more common in adults over 50.

Cervical Foraminal Stenosis
Foraminal stenosis is a narrowing of the bony canal through which the nerve root exits the spinal column. It can result from a combination of degenerative disc disease, bone spur formation, thickening of the ligamentum flavum, and hypertrophy of the facet joints. When the foramen becomes too narrow, the nerve root inside is persistently compressed, producing chronic radicular symptoms that are typically position-dependent and aggravated by activities that reduce foraminal space.
Trauma and Acute Injuries
Traumatic events such as whiplash, contact sports injuries, falls, or motor vehicle accidents can cause acute disc herniations, vertebral fractures, or ligamentous injuries that compress cervical nerve roots. Post-traumatic radiculopathy may develop immediately after the injury or appear weeks to months later as swelling and inflammation evolve.
Postural and Occupational Factors
Prolonged poor posture, particularly forward head posture commonly associated with extensive computer use and smartphone use, places increased mechanical stress on the cervical discs and joints. Over time, this contributes to disc degeneration and may accelerate the development of foraminal narrowing. Occupations that require repetitive overhead work, prolonged seated postures, or heavy lifting without proper technique are also recognized risk factors for cervical radiculopathy.
How Is a Pinched Nerve in the Neck Diagnosed?
Accurate diagnosis requires a combination of clinical evaluation and imaging studies. At Deuk Spine Institute, our diagnostic approach is thorough and tailored to each patient's source of pain.
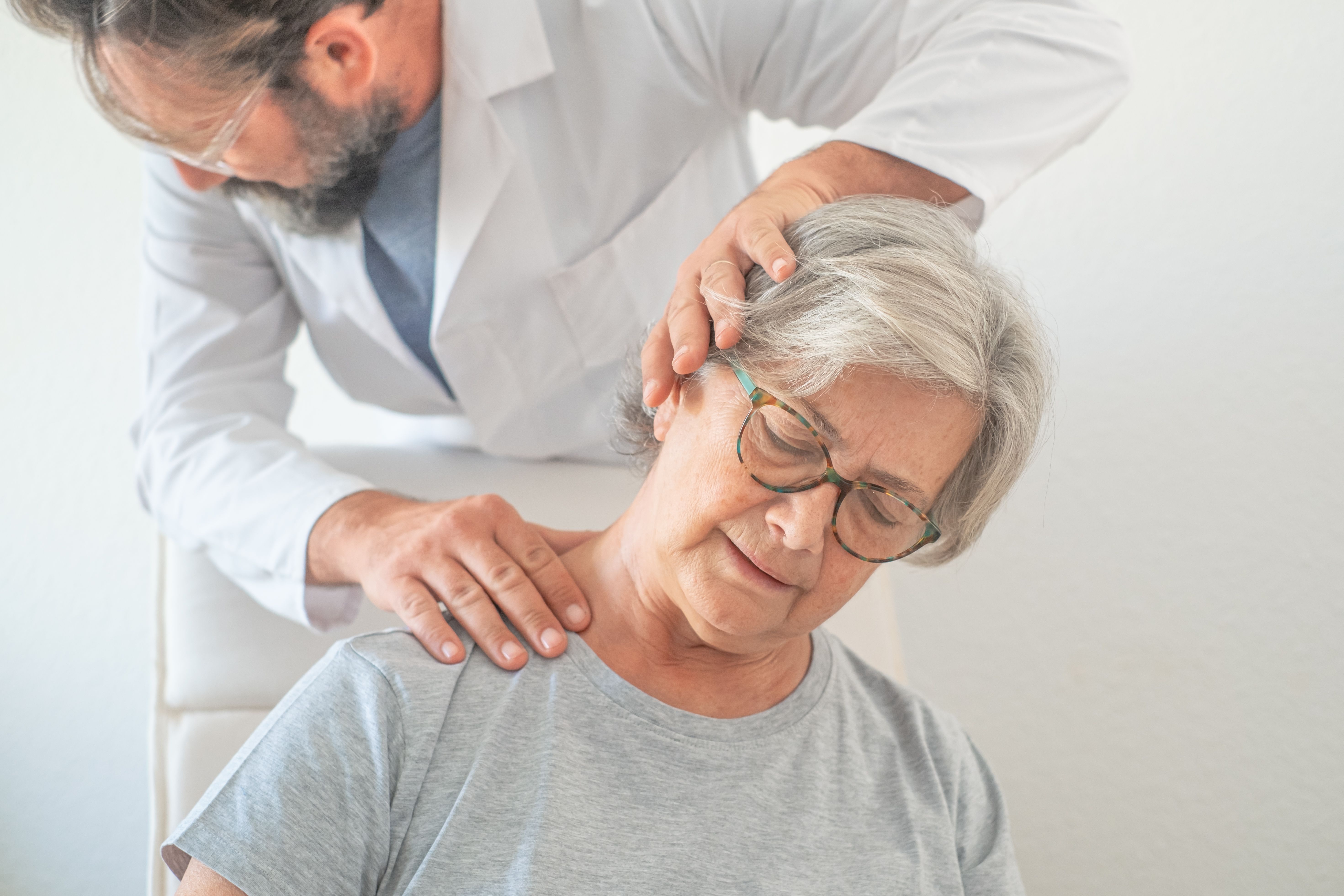
Clinical History and Physical Examination
The diagnostic process begins with a detailed history of your symptoms, their onset, distribution, aggravating and relieving factors, and how they have changed over time. The physical examination includes assessment of cervical range of motion, palpation of the cervical spine and surrounding musculature, and a targeted neurological exam to evaluate sensation, motor strength, and deep tendon reflexes in both arms.
Provocative tests such as the Spurling compression test (applying downward pressure on the head while tilted toward the symptomatic side) and the upper limb tension test are used to reproduce radicular symptoms and help confirm the diagnosis. A 2025 scoping review in BMC Musculoskeletal Disorders found that combining multiple components of the neurological examination yielded the highest diagnostic specificity for cervical radiculopathy.
MRI of the Cervical Spine
Magnetic resonance imaging (MRI) is the preferred imaging modality for evaluating a suspected pinched nerve in the neck. MRI provides detailed soft tissue visualization, allowing the physician to identify the exact level and cause of nerve root compression, whether from a herniated disc, bone spur, or foraminal stenosis. It also reveals the degree of nerve root impingement and any associated changes in the spinal cord.
Submitting your existing MRI for a free review by Dr. Ara Deukmedjian at Deuk Spine Institute can provide valuable clarity about your diagnosis and available treatment options. A free 10-minute virtual consultation could change everything.
CT Myelography
In some cases, particularly when MRI is not feasible or when bony detail is required, computed tomography (CT) myelography may be used. This involves injecting contrast dye into the spinal canal and then performing CT imaging to visualize the nerve roots and any compressive pathology. A 2024 update on cervical radiculopathy imaging published in the Journal of the American College of Radiology confirmed that CT with contrast myelography remains a high-value imaging tool when MRI results are inconclusive. 3

Electrodiagnostic Testing
Electromyography (EMG) and nerve conduction studies (NCS) can provide objective confirmation of nerve root dysfunction and help distinguish radiculopathy from peripheral nerve conditions such as carpal tunnel syndrome. EMG assesses the electrical activity of muscles supplied by the affected nerve root, while NCS measures the speed and amplitude of electrical signals along peripheral nerves. These tests are particularly useful when the clinical picture is unclear or when multiple levels of involvement are suspected.
Non-Surgical Treatment Options
For many patients, a pinched nerve in the neck improves significantly with conservative care, particularly when symptoms are mild to moderate and have been present for a relatively short time.

Physical Therapy
A structured physical therapy program is typically the foundation of conservative treatment for cervical radiculopathy. Therapeutic exercises targeted at the cervical and upper thoracic spine can improve posture, restore normal movement mechanics, reduce muscle guarding, and decrease the load on compromised nerve roots. Manual therapy techniques, including cervical joint mobilization and soft tissue work, can also reduce pain and improve range of motion. A 2025 network meta-analysis published in PMC found that manual therapy combined with traction produced meaningful reductions in neck disability scores and pain in patients with cervical radiculopathy. 4
Cervical Traction
Cervical traction applies a gentle distracting force to the neck, separating the vertebrae and temporarily increasing foraminal space. This can reduce direct mechanical pressure on a compressed nerve root and provide significant short-term pain relief. Traction may be performed mechanically in a clinical setting or at home with a prescribed device under physician guidance.
Medications
Several medication classes are used to manage the pain and inflammation associated with cervical radiculopathy. Nonsteroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen or naproxen reduce inflammation around the compressed nerve root. Short courses of oral corticosteroids may be prescribed for acute, severe radicular pain. Gabapentinoids such as gabapentin or pregabalin help modulate neuropathic pain signals. Muscle relaxants may be useful when significant muscle spasm is contributing to symptoms. All medications should be used under the supervision of a physician, and long-term use of opioid analgesics is generally not recommended for cervical radiculopathy.

Cervical Epidural Steroid Injections
For patients who do not respond sufficiently to oral medications and physical therapy, cervical epidural steroid injections can deliver anti-inflammatory corticosteroids directly to the area surrounding the compressed nerve root. This targeted approach can reduce nerve root inflammation and provide significant pain relief for weeks to months. Injections are typically considered a bridge to allow participation in physical therapy rather than a permanent solution.
Activity Modification and Postural Correction
Adjusting daily habits and work ergonomics can significantly reduce mechanical stress on the cervical spine. Positioning your computer monitor at eye level, using a headset rather than cradling a phone between the ear and shoulder, taking frequent breaks from sustained postures, and sleeping with a supportive cervical pillow are all practical measures that can reduce symptom aggravation during recovery.

When Is Surgery Needed for a Pinched Nerve in the Neck?
Surgery is recommended when conservative measures have failed to provide adequate relief after an appropriate trial of care, when neurological deficits such as muscle weakness or reflex loss are progressing, or when symptoms are severe enough to significantly impair daily function or quality of life.
A 2024 prospective multicenter study published in Scientific Reports, which analyzed 359 patients undergoing single-level cervical decompression surgery, found that arm pain was reduced by an average of 3.4 points on the numerical rating scale following surgery, with meaningful improvement across all cervical levels treated. The study also found that patients with C8 radiculopathy tended to have more complex outcomes, highlighting the importance of level-specific surgical planning.
Deuk Laser Disc Repair® at Deuk Spine Institute
For patients whose radiculopathy is caused by a herniated or damaged cervical disc, Deuk Spine Institute offers Deuk Laser Disc Repair®, a proprietary minimally invasive endoscopic procedure developed by Dr. Ara Deukmedjian.
Unlike traditional open cervical surgery, Deuk Laser Disc Repair® is performed through a 4mm opening using an endoscope and a specialized laser. The procedure directly targets the source of nerve compression by treating the damaged disc tissue and eliminating the inflammation that is irritating the nerve root. There is no hardware, no bone grafting, no fusion, and no overnight hospital stay. Most patients walk out of the clinic the same day the procedure is performed.
The procedure is indicated for patients with disc herniations, bulging discs, or related disc pathology confirmed on MRI. Patients with significant bone spur-based stenosis may require evaluation for alternative surgical approaches. A consultation with Dr. Deukmedjian will clarify whether Deuk Laser Disc Repair® is appropriate for your specific anatomy and diagnosis.
Patient Spotlight: A Military Veteran Chooses DLDR® Over Fusion
Sometimes the best way to understand what a procedure means in practice is to hear from someone who lived it. A military veteran from California arrived at Deuk Spine Institute with herniated discs at C5-6 and C6-7 that had been building for years, the result of a lifetime of physical trauma that began in childhood and intensified through years of military service, parachute jumps, and the sustained weight of wearing Kevlar helmets in the field. By the time he sought treatment, the tingling in his left arm had become constant and debilitating.
He had already done his homework before arriving. Disc replacement was one option, but the idea of implanting a metal prosthetic that was never designed for his spine did not sit well with him. Anterior cervical discectomy and fusion (ACDF) was another, but his own mother had undergone lumbar fusion and suffered significant complications over time. He kept searching until he found Deuk Spine Institute.
Less than 24 hours after undergoing Deuk Laser Disc Repair® for both disc levels, he described a quality of relief he had not experienced in over a decade: "It's a sort of ease that I haven't had probably for more than 10 years at least." The radiating arm pain, the electric tingling, the constant tension that had shadowed his daily life were gone. He walked out of the clinic the same day his procedure was performed, without metal implants, without a hospital stay, and without the movement restrictions that come with fusion.
His story reflects what Dr. Deukmedjian has observed across thousands of patients: when the source of nerve compression is treated directly and precisely, the results can be immediate and profound. For patients who have been told that fusion or disc replacement is their only path forward, Deuk Laser Disc Repair® offers a fundamentally different option, one that addresses the damaged disc without altering the mechanics of the spine.
Red Flags: When to Seek Immediate Medical Attention
While most cases of cervical radiculopathy are not medical emergencies, certain symptoms require urgent evaluation. You should seek immediate medical attention if you experience any of the following:
- Rapidly progressive weakness in the arm or hand
- Loss of coordination or difficulty walking
- Bowel or bladder dysfunction (including incontinence or retention), which may indicate cervical myelopathy (spinal cord compression)
- Severe pain following trauma to the head or neck
- Symptoms that develop in the context of fever, unexplained weight loss, or a history of cancer
These presentations may indicate spinal cord involvement or another serious underlying condition that requires prompt diagnosis and treatment.
Living With a Pinched Nerve in the Neck: What to Expect
The natural history of cervical radiculopathy is generally favorable for many patients, with symptoms improving over several weeks to months in mild to moderate cases. However, this improvement is not guaranteed, and the risk of symptom recurrence or progression to more severe neurological deficits is real, particularly if the underlying cause is not addressed.
Patients who achieve resolution of symptoms through conservative care should continue with the lifestyle habits and postural practices that supported their recovery. Ongoing cervical strengthening, postural awareness, and ergonomic management are key to reducing the risk of recurrence.
For patients who require surgical treatment, recovery from Deuk Laser Disc Repair® is typically rapid. Because the procedure is performed on an outpatient basis with a minimal incision, most patients return to light activities within days and resume a fuller range of activity within weeks, far sooner than the recovery timeline associated with traditional open cervical surgery.
Take the First Step Toward Pain-Free Living
A pinched nerve in the neck is not something you need to simply endure. Whether your symptoms are new or have been troubling you for years, an accurate diagnosis is the foundation for effective relief. The physicians at Deuk Spine Institute, led by Board-Certified Neurosurgeon Dr. Ara Deukmedjian, bring decades of specialized spine care experience to every patient evaluation.
You can submit your MRI for a FREE review and receive a 10-minute virtual consultation with Dr. Deukmedjian to discuss your imaging findings and treatment options. There is no cost, no obligation, and no reason to keep waiting.
Frequently Asked Questions
Q: How do I know if my neck pain is from a pinched nerve or just muscle strain?
A: Muscle strain typically causes localized pain in the neck that resolves within a few days to two weeks with rest and gentle movement. A pinched nerve produces pain that radiates from the neck into the shoulder, arm, or fingers, often following a specific path. It is also frequently accompanied by tingling, numbness, or weakness in the arm, none of which are typical features of muscle strain. If your pain radiates beyond the neck or you notice any neurological symptoms in your arm or hand, you should see a physician for evaluation rather than assuming it will resolve on its own.
Q: Can a pinched nerve in the neck heal on its own?
A: In mild to moderate cases, cervical radiculopathy can improve substantially over a period of weeks to months with conservative care, including physical therapy, activity modification, and appropriate pain management. However, improvement without treatment is not guaranteed, and symptoms that are severe, progressively worsening, or accompanied by motor weakness require medical evaluation. Waiting too long to seek treatment can allow nerve damage to become permanent, particularly when disc herniation or foraminal stenosis is the underlying cause. Early diagnosis gives you the best opportunity for full recovery.
Q: What makes Deuk Laser Disc Repair® different from traditional cervical surgery?
A: Traditional anterior cervical discectomy and fusion (ACDF) involves removing the disc, inserting hardware such as a cage and screws, and fusing the adjacent vertebrae together. This requires a visible incision, hardware implantation, and often an overnight hospital stay, followed by several weeks of restricted activity. Deuk Laser Disc Repair® is performed endoscopically through a 4mm portal, treats the damaged disc directly without hardware or fusion, and is completed as an outpatient procedure. Patients typically walk out of the clinic the same day. The procedure preserves the natural motion of the cervical spine and avoids the adjacent segment stress that can accompany fusion procedures.
Q: How long does it take to recover from a pinched nerve in the neck?
A: Recovery depends on the severity and duration of nerve compression, the treatment approach used, and individual patient factors. Patients treated conservatively may see gradual improvement over four to twelve weeks. Patients who undergo Deuk Laser Disc Repair® typically resume light activity within days of the procedure. Full recovery from more significant nerve compression can take longer, particularly if the nerve was compressed for an extended period before treatment began. The sooner the underlying cause is identified and addressed, the faster and more complete the recovery tends to be.