Procedure Not Recommended
Risks, Complications & Better Alternatives

⚠️ While Deuk Spine Institute can perform Laminectomy, we do not recommend it. This page explains why — learn the risks before consenting to this procedure.
UNDERSTANDING THE PROCEDURE
While there are legitimate medical reasons, financial incentives often influence surgical recommendations.
Nerve compression causing radiating pain and numbness. However, laminectomy rarely addresses the actual inflammation source.
Severe leg pain from compressed nerves. Laminectomy destroys stabilizing structures while leaving the herniated disc untreated.
Canal narrowing causing cord compression. Surgeons often overdiagnose this on MRI to justify laminectomy for mild cases.
Rare emergency (<1% of stenosis cases) often used to justify laminectomy for much less severe conditions.
Among the highest-reimbursed spine surgeries, creating powerful financial incentive even when less invasive options exist.
Extended operating time, overnight stays, and complex post-surgical care drive massive hospital revenue.
Laminectomy destroys stabilizing bone and ligaments, causing instability that guarantees repeat procedures.
Failed laminectomies create patients needing ongoing injections, ablations, stimulators, and opioids for life.
Success rate for eliminating chronic back pain is under 20%, yet it continues generating substantial revenue.
Surgeons receive the same compensation whether pain resolves or worsens. The system rewards volume, not results.
THE SURGICAL PROCESS
The videos below contain real surgical footage. Viewer discretion is advised.
A 3–6 inch incision is made along the spine to expose the underlying structures.
The tough connective tissue covering the spine muscles is cut and removed.
Spinal muscles are stripped from the bone, causing permanent damage and weakness.
The bony protrusion at the back of each vertebra is cut away with surgical instruments.
The lamina (protective bone arch) is removed, exposing the spinal cord and nerves.
Facet joints that provide spinal stability are destroyed, often leading to instability.
CRITICAL RISKS
20 documented reasons with supporting images and surgical footage.
Images and videos below contain real surgical procedures and medical imagery.
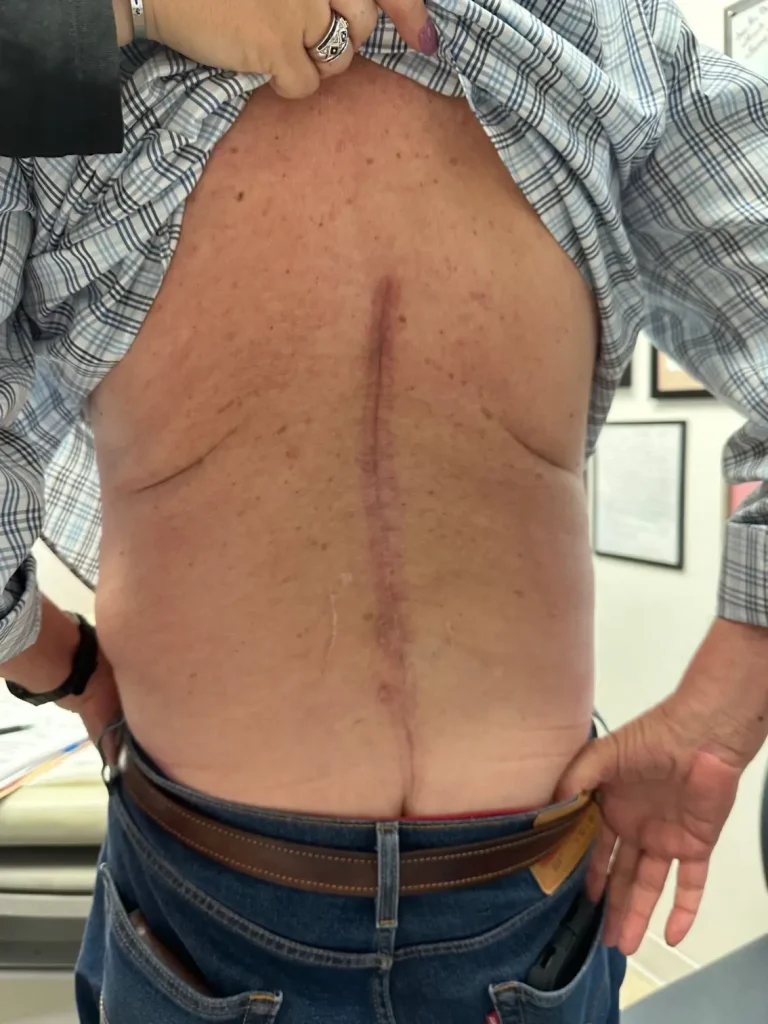
Highly invasive: large incision and excessive cutting of normal tissues between skin and spine during laminectomy.
Excessive and unnecessary bleeding during and after surgery from muscle trauma by the surgeon.
Destruction of normal stabilizing bones including lamina and spinous process by the surgeon during laminectomy.
Destruction of normal stabilizing bones including lamina and spinous process by the surgeon during laminectomy.
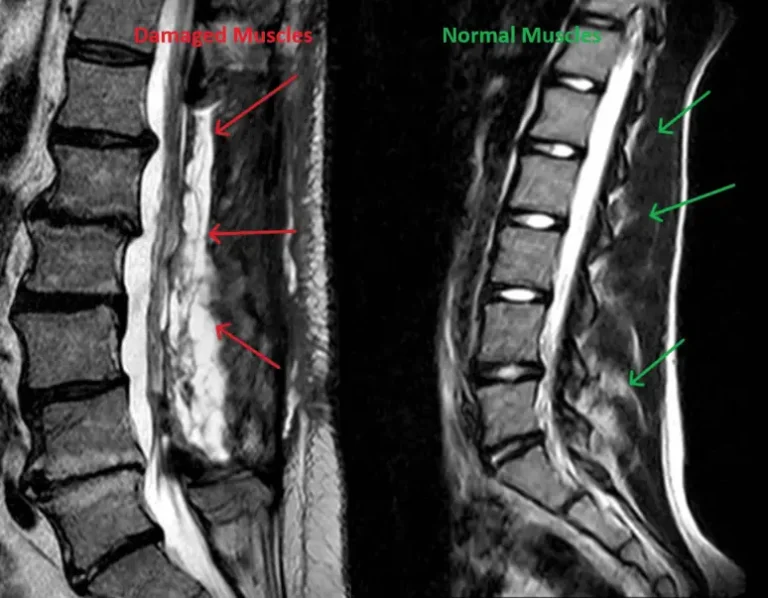
Destruction of normal stabilizing bones including lamina and spinous process by the surgeon during laminectomy.
Excessive scar tissue forms around the spine and nerves after laminectomy
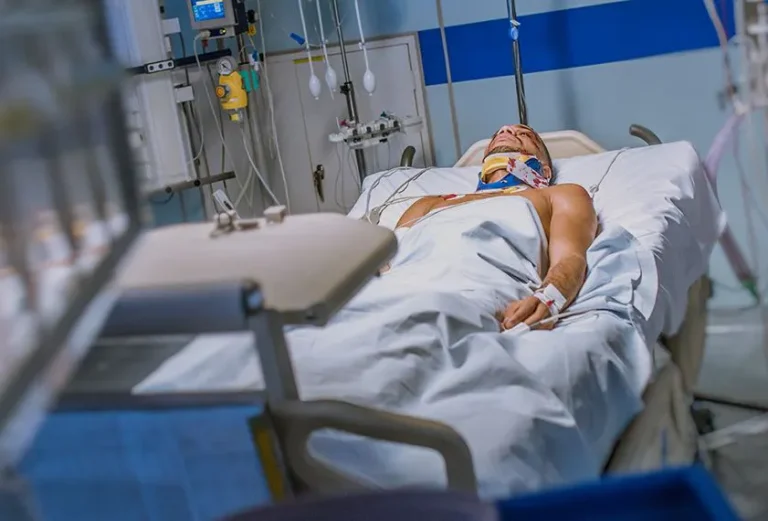
Complications are common after laminectomy
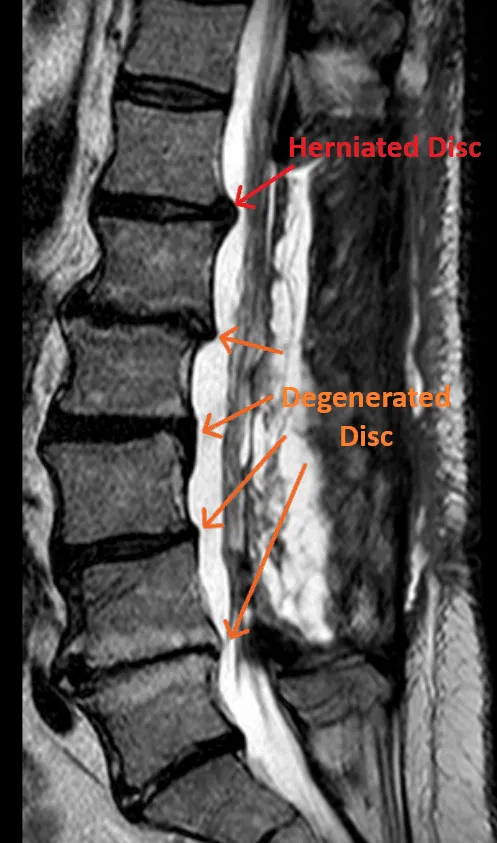
Disc herniations and degenerated discs are not treated when a laminectomy is performed. They are the most common cause of back and leg pain.
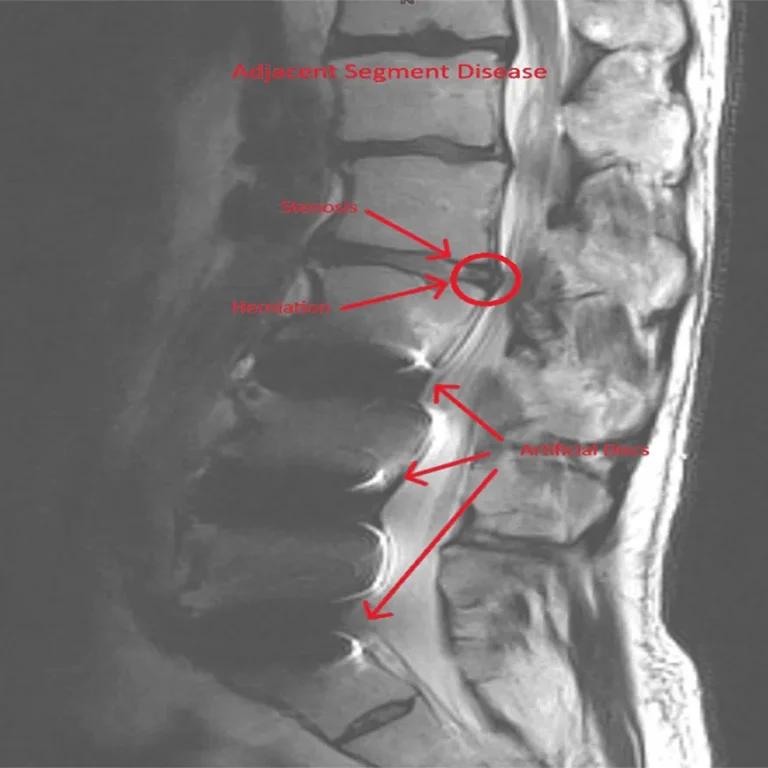
Adjacent segment disease is common after laminectomy and requires additional surgery.
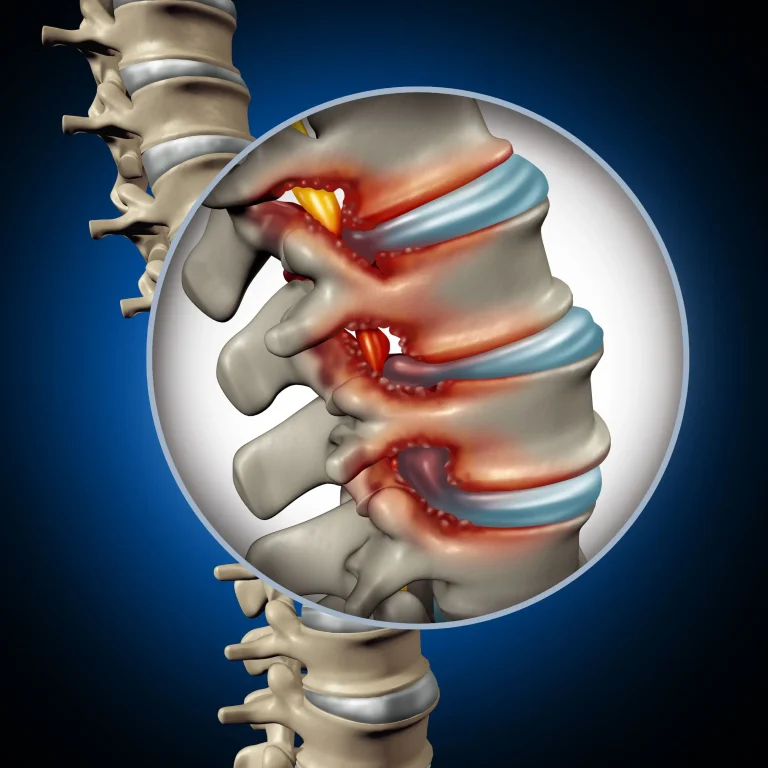
Stenosis either persists or reoccurs commonly after laminectomy and will require additional surgery such as Fusion.
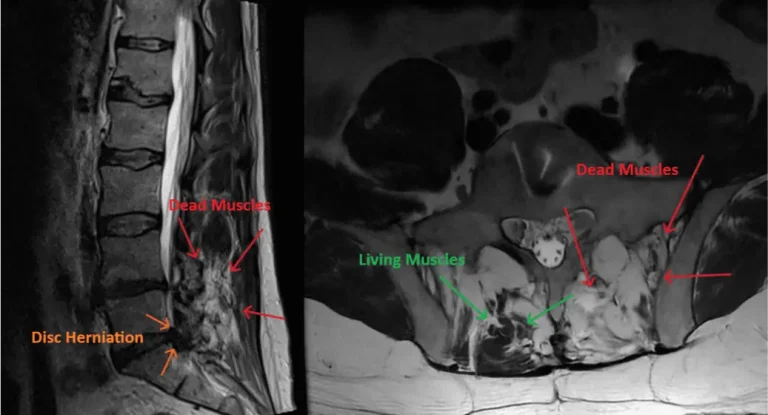
Excessive postoperative pain always occurs after laminectomy due to muscle trauma and necrosis (death of muscles). During laminectomy the muscles are torn off the spine by the surgeon in order to get down to the lamina. The dying muscles cause severe postoperative pain that always requires opioid painkillers and muscle relaxers. Opioid painkillers are highly addicting, cause tolerance, abuse and even death from breathing failure.
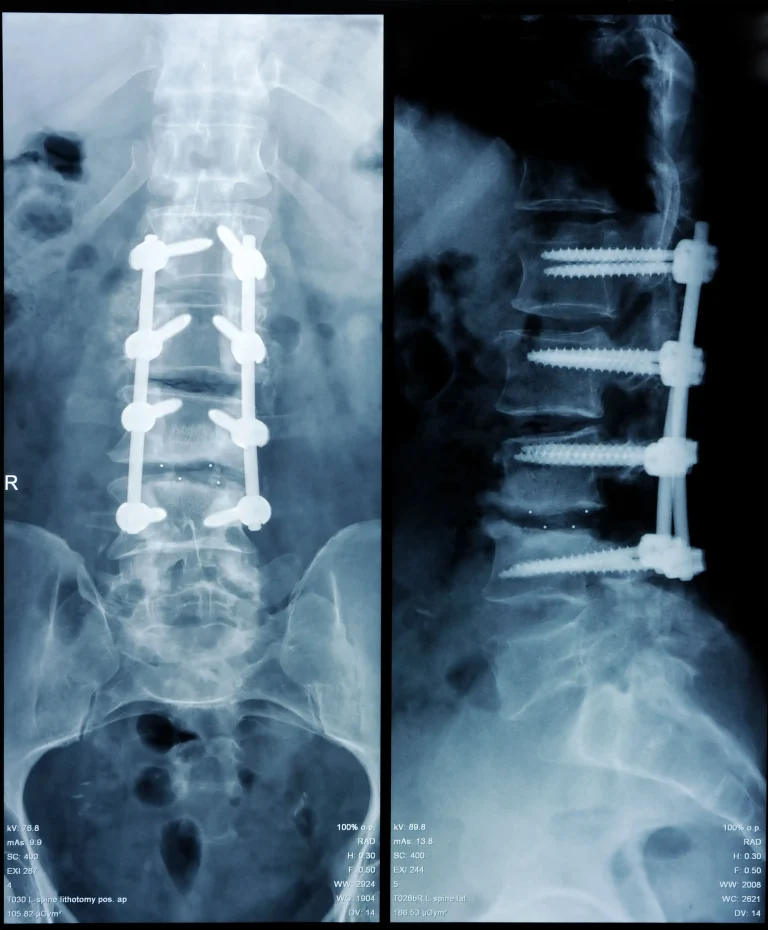
Back pain becomes worse after laminectomy. Fusion will be recommended.
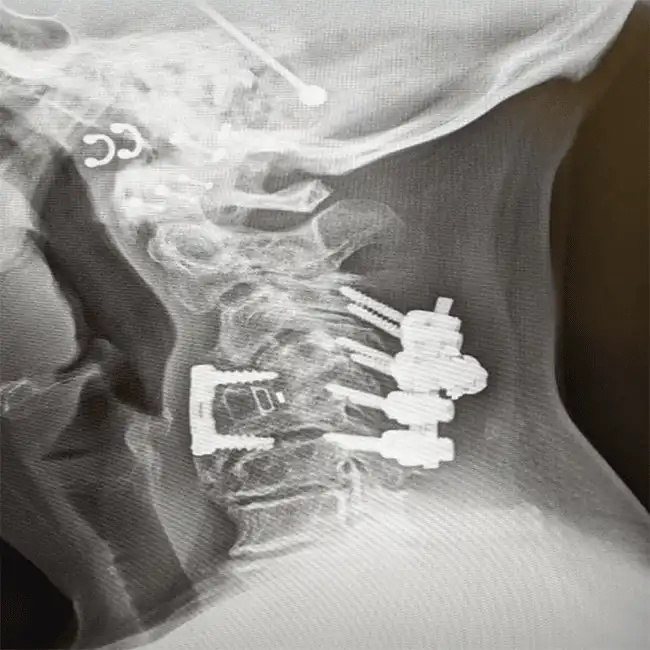
Destruction of normal stabilizing bones including lamina and spinous process by the surgeon during laminectomy.

Long operating times are needed for laminectomy.
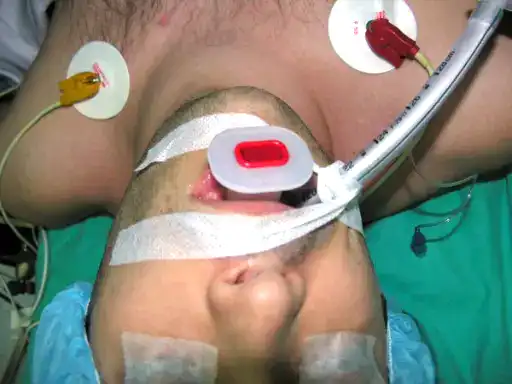
General intubated anesthesia is needed for laminectomy.
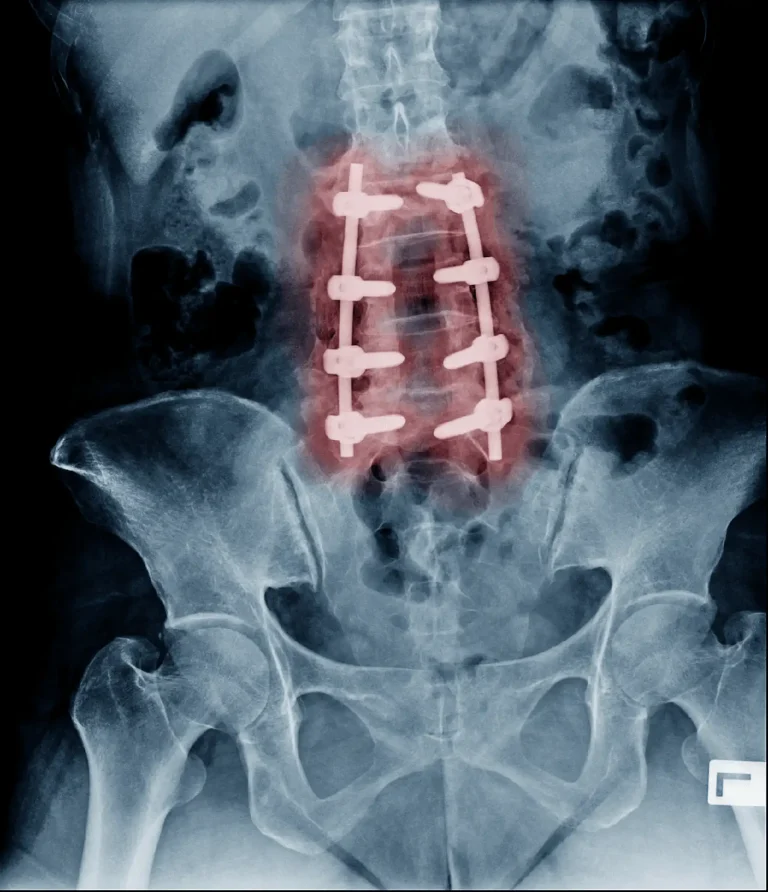
Additional surgery will be necessary in over 90% of patients having laminectomy.
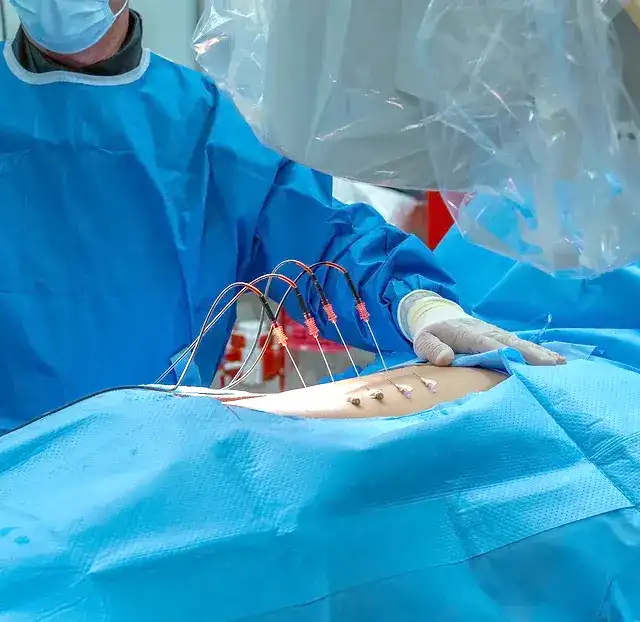
Most laminectomy patients end up in pain management for years after laminectomy.
DOCUMENTED COMPLICATIONS
Images and videos below contain real surgical procedures and medical imagery.
Permanent nerve damage causing weakness, numbness, or paralysis in extremities.
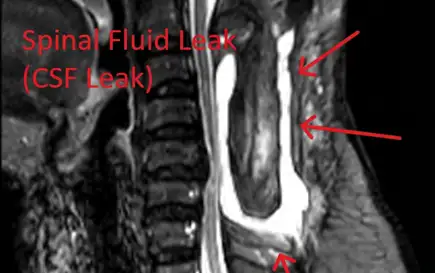
Dural tears leading to cerebrospinal fluid leaks, requiring additional repair surgery.
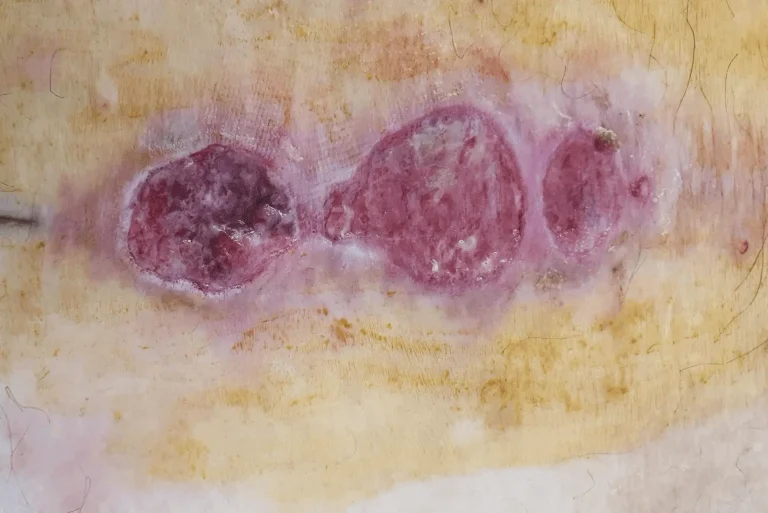
Post-surgical infection at the incision site or deeper within the spinal structures.
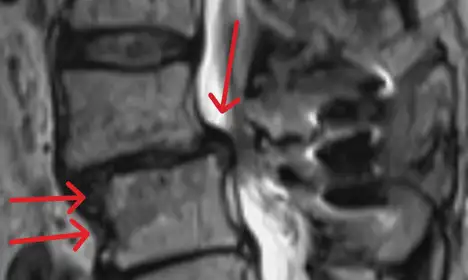
Removal of stabilizing structures causes instability requiring fusion with screws and rods.
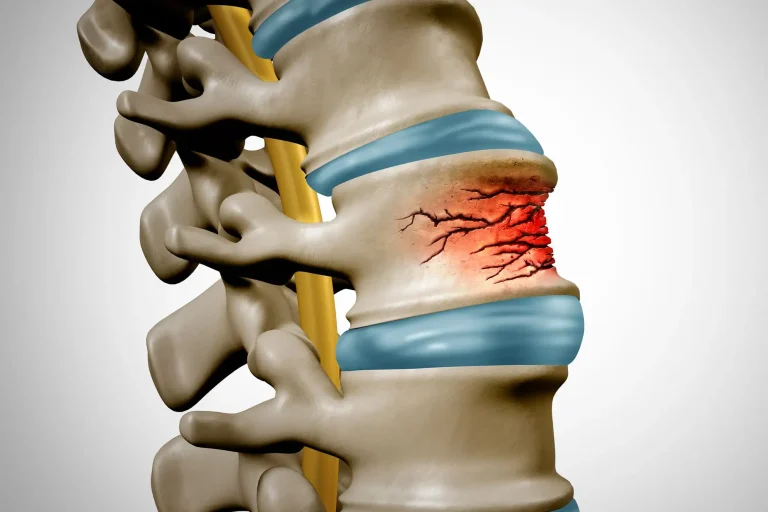
Weakened spine from bone removal can lead to vertebral fractures and collapse.
Stenosis persists or reoccurs commonly after laminectomy, requiring additional surgery.
WHAT WE RECOMMEND INSTEAD
Instead of destroying your spine’s stabilizing structures, Deuk Laser Disc Repair® uses endoscopic technology and laser precision to treat the actual source of pain — the damaged disc — through an incision smaller than a fingernail.
Your spine’s stabilizing structures remain completely intact. No lamina, spinous process, or facet joint destruction.
Laser technology directly repairs the damaged disc — the actual source of 85% of chronic back pain that laminectomy ignores.
Outpatient procedure under light sedation. Walk out the same day — no hospital stay, no intubation, no opioids required.
95% patient satisfaction, 0.01% complication rate, and over 1,300 successful procedures performed by Dr. Deukmedjian.
Feature
Laminectomy
Deuk Laser Disc Repair®
Procedure Type
❌ Highly invasive, open surgery
✅ Minimally invasive, endoscopic
Incision Size
❌ 3–6 inches
✅ Less than 1/4 inch
Anesthesia
❌ General (intubated)
✅ Light IV sedation
Bone Removal
❌ Yes — lamina & spinous process
✅ None
Treats Disc Injury
❌ No — disc left untreated
✅ Yes — laser repairs the disc
Hospital Stay
❌ 1–3 days inpatient
✅ Outpatient — go home same day
Recovery Time
❌ 6–12 weeks
✅ Days
Complication Rate
❌ High — frequent complications
✅ 0.01%
Success Rate
❌ Less than 20%
✅ 95% patient satisfaction
Repeat Surgery
❌ 40–50% need fusion in 5 years
✅ Rarely needed
A BETTER ALTERNATIVE
Minimally invasive, outpatient procedure with a 0.01% complication rate and 95% patient satisfaction. No bone removal. No muscle destruction. Same-day recovery.
Patient Satisfaction
Complication Rate
Procedure Time