By Dr. Ara Deukmedjian, MD
Board-Certified Neurosurgeon, Deuk Spine Institute
Medically reviewed on April 2, 2026
Medical Disclaimer: This content is for educational purposes only and does not constitute medical advice. Individual results may vary. Always consult with your healthcare provider about your specific condition and treatment options.
Key points
✓ Spine pain can come from discs, joints, muscles, ligaments, nerves, posture, injury, or degenerative changes.
✓ Many cases improve with conservative care such as activity modification, physical therapy, exercise, and lifestyle changes.
✓ Recent evidence and guideline updates show that some common injection-based procedures offer little benefit for chronic axial spine pain and should be used selectively.
✓ Exercise-based care remains one of the most consistently supported approaches for chronic low back pain, with recent reviews continuing to show benefit.
✓ Surgery may be appropriate in selected cases when a structural problem clearly matches the symptoms and non-surgical care has not helped.

What Is Spine Pain?
Spine pain is discomfort that starts in or around the spinal column, which includes the cervical, thoracic, and lumbar regions. 1 It may be felt locally in the neck or back, or it may radiate into the arms, buttocks, or legs when nerves are irritated or compressed.
The spine is essential for support, motion, and protection of the spinal cord. When a spinal structure becomes inflamed, strained, compressed, or injured, pain can limit daily activities such as sitting, standing, walking, sleeping, and lifting.
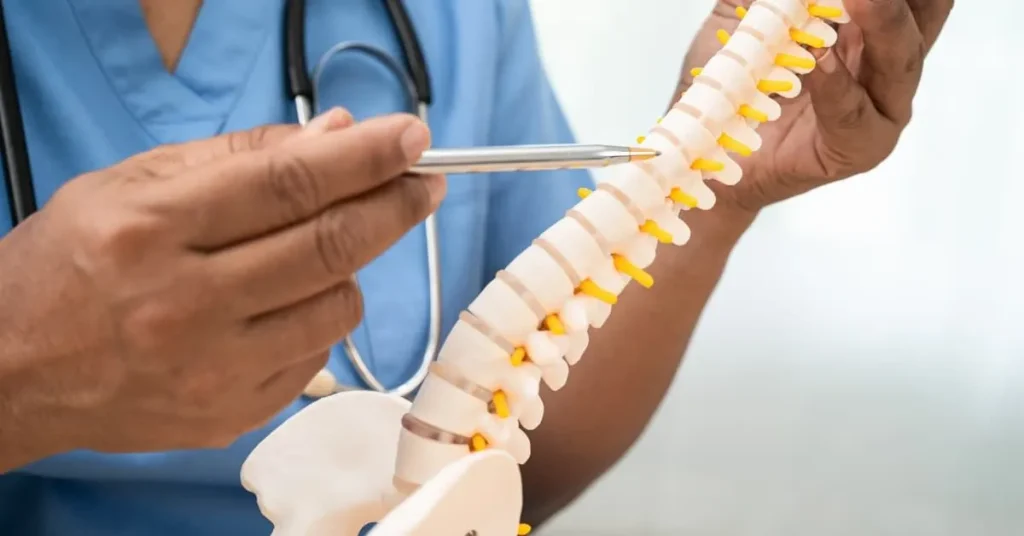
How Spine Pain Develops
Spine pain is often multifactorial, which means more than one tissue can be involved. Common pain generators include discs, facet joints, muscles, ligaments, nerves, and the sacroiliac joints.
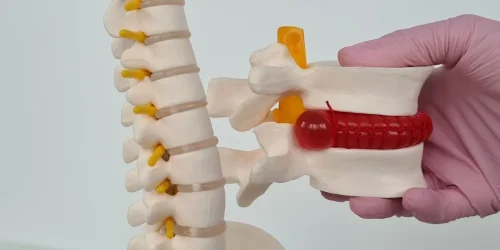
In disc-related pain, an injury or wear-and-tear change can lead to an annular tear, disc bulge, or herniation. The disc material may irritate nearby inflammatory tissues and nerve roots, which can create localized back pain or pain that travels down a leg or arm. However, a disc abnormality on imaging does not always mean it is the cause of the pain.
Spine Regions
The spine is commonly divided into three regions:
- Cervical spine, or neck.
- Thoracic spine, or upper and middle back.
- Lumbar spine, or lower back.
The thoracic spine tends to be stiffer than the cervical and lumbar regions, so it is less commonly injured by routine motion, though it can still be a source of pain.
Common Causes
Many conditions can contribute to spine pain. Some of the most common include:
- Muscle strain from lifting, twisting, poor posture, or prolonged sitting.
- Ligament sprain from overstretching or sudden movement.
- Degenerative disc disease or disc herniation.
- Facet joint arthritis.
- Spinal stenosis.
- Scoliosis or kyphosis.
- Osteoporosis and compression fractures.
- Inflammatory conditions such as ankylosing spondylitis.
- Infection, tumor, or spinal cord injury in less common but more serious cases.
A 2025 Scientific Reports study found that people with chronic low back pain performed significantly fewer lumbar movements over a 24-hour period than asymptomatic individuals, which supports the idea that chronic pain is often linked with guarded movement and reduced mobility. 4
Symptoms To Watch For
Spine pain can present in different ways depending on the source and severity. Common symptoms include:
- Pain in the neck, mid back, or low back.
- Pain that radiates into the buttocks, hips, arms, or legs.
- Stiffness or reduced range of motion.
- Muscle spasms.
- Weakness or fatigue.
- Poor posture or difficulty standing upright.
- Pain that worsens with sitting, bending, lifting, or twisting.
Some symptoms should never be ignored. Seek urgent medical care if spine pain is associated with:
- Bowel or bladder changes.
- Fever or chills.
- Numbness in the groin or saddle area.
- Sudden weakness.
- Pain after a fall, accident, or other injury.
How Spine Pain Is Evaluated
A careful diagnosis matters because treatment should match the pain generator, not just the location of pain. Clinicians typically review the patient’s history, symptoms, physical exam findings, and imaging if needed.
Important questions include whether the pain is mechanical, inflammatory, nerve-related, or related to injury. In many cases, imaging findings must be interpreted cautiously because common age-related changes can appear even in people without pain. Learn more about ways to manage chronic back pain.

Non-Surgical Treatment
For many patients, conservative care should be the first step. Recent research continues to support exercise-based care and movement-focused treatment as important tools for chronic low back pain. 2
Physical Therapy
Physical therapy is often one of the first treatment options for spine pain. A well-designed program may include stretching, strengthening, mobility work, posture training, and education on how to move safely during daily activities.
The goal is to reduce pain, restore function, and lower the risk of recurrence. Recent exercise research continues to show that structured activity can improve pain and function in chronic low back pain, especially when it is performed consistently over time.
Exercise And Movement
Exercise is one of the most evidence-supported approaches for chronic spine pain. A 2025 network meta-analysis found that exercise interventions meaningfully reduced pain, and that programs such as Tai Chi, yoga, Pilates, walking, core training, and stretching can all help depending on the patient and presentation.

This matters because chronic spine pain often leads people to move less, which can worsen stiffness and loss of function. The best program is usually individualized and progressed gradually so the patient can move with less fear and better control.
Mindfulness And Stress Reduction
Mindfulness and meditation can be useful adjuncts, especially when pain is persistent and stress levels are high. They do not fix the structural cause of pain, but they may reduce pain amplification, muscle guarding, and the emotional burden that often accompanies chronic back pain.
Nutrition And Lifestyle
Healthy weight management, smoking cessation, better sleep, and regular activity can all support spine health. While diet alone is not a cure, maintaining good nutrition may help overall recovery and inflammation control, especially when paired with movement-based treatment.

Injection-Based Treatments
Injection-based procedures are sometimes used when symptoms suggest a specific pain source such as a nerve root, joint, or inflamed disc. However, the evidence is mixed, and these procedures should not be presented as a universal solution for chronic spine pain.
The BMJ’s 2025 guideline issued strong recommendations against several commonly used injection and ablation procedures for chronic spine pain because they provide little or no meaningful benefit compared with other treatments in many cases. 3 That does not mean injections are never appropriate, but it does mean they should be selected carefully and discussed honestly with patients.
Procedures sometimes considered include:
- Epidural steroid injection.
- Facet joint injection.
- Medial branch block.
- Radiofrequency ablation.
- Selective nerve root block.
- Sacroiliac joint injection.
When Surgery May Be Considered
Surgery is not the first choice for most back pain. It is usually considered when a clear structural problem matches the patient’s symptoms, and when conservative treatment has not produced sufficient improvement.
Surgery may be more appropriate when there is:
- Persistent nerve compression.
- Progressive weakness.
- A structural lesion that clearly matches the pain pattern.
- Severe disability despite appropriate non-surgical care.
A 2025 evidence-based review of current surgical treatments for lumbar degenerative disease highlights the importance of matching the procedure to the pathology and patient goals rather than assuming one operation fits every type of pain. 5
Surgical Options
If surgery is needed, the choice depends on the cause of pain. Options may include discectomy, decompression, laminectomy, foraminotomy, disc replacement, fusion, or other minimally invasive procedures depending on anatomy and symptoms. At Deuk Spine Institute, we always recommend the Deuk Laser Disc Repair whenever it can effectively address the root cause of your back pain.
Deuk Laser Disc Repair®
For patients with chronic back or neck pain caused by disc-related conditions, there are several treatment options available. In some cases, when conservative treatments such as physical therapy, medications, or injections do not provide enough relief, a minimally invasive surgical approach may be considered.
Deuk Laser Disc Repair® is an endoscopic, minimally invasive spine procedure performed at Deuk Spine Institute for carefully selected patients with disc injuries, such as herniated or bulging discs.
This technique was developed by Dr. Ara Deukmedjian and focuses specifically on treating pain that originates from damaged spinal discs.
How the Procedure Works
Deuk Laser Disc Repair®(DLDR) is performed through a very small incision using advanced endoscopic technology. A specialized camera allows the surgeon to directly visualize the affected disc and surrounding structures in real time.
Using a laser, the surgeon carefully removes inflamed or damaged disc material that may be contributing to pain. This targeted approach is designed to address the source of disc-related pain while minimizing disruption to nearby muscles and tissues.
Because the procedure is performed endoscopically patients can go home the same day.
Recovery And Prevention
Recovery depends on the cause of pain and the treatment used. Most patients do better when they stay appropriately active, follow a personalized exercise plan, and avoid long periods of bed rest unless advised otherwise.
Prevention strategies include:
- Maintaining good posture.
- Using proper lifting mechanics.
- Avoiding tobacco use.
- Keeping a healthy body weight.
- Exercising the core, hips, and back regularly.
- Managing stress and sleep quality.
When To See A Specialist
You should see a spine specialist when pain lasts longer than expected, keeps returning, or interferes with work, sleep, or daily life. You should seek urgent evaluation sooner if symptoms suggest nerve damage, spinal instability, infection, fracture, or another serious condition.

FAQs
Q: What causes spine pain most often?
A: The most common causes are muscle strain, disc problems, arthritis, poor mechanics, and degenerative changes. Nerve irritation, inflammation, and posture-related overload are also frequent contributors.
Q: Is exercise safe for spine pain?
A: For most people, yes. Recent evidence continues to support exercise as one of the most effective non-surgical treatments for chronic low back pain, especially when it is individualized and progressed gradually.
Q: Are spine injections always helpful?
A: No. A 2025 BMJ guideline found that several commonly used injections and ablation procedures offer little or no meaningful benefit for many adults with chronic axial spine pain.
Q: When is surgery necessary?
A: Surgery may be considered when there is a clearly identified structural problem, such as nerve compression or instability, and symptoms persist despite appropriate conservative care.
Sources
- Cleveland Clinic, Spine structure and function: https://my.clevelandclinic.org/health/articles/10040-spine-structure-and-function
- The BMJ, Commonly used interventional procedures for non-cancer chronic spine pain: https://www.bmj.com/content/388/bmj-2024-079970
- BMJ Group press release, Experts strongly recommend against spine injections for chronic back pain: https://bmjgroup.com/back-pain-recommendations/
- Nature Scientific Reports, Chronic low back pain is associated with a reduction in lumbar movement: https://www.nature.com/articles/s41598-025-04851-2
- PubMed, An evidence-based review of the current surgical treatments for lumbar degenerative disease: https://pubmed.ncbi.nlm.nih.gov/39919297/