By Dr. Ara Deukmedjian, MD
Board-Certified Neurosurgeon, Deuk Spine Institute
Medically reviewed on March 12, 2026
Medical Disclaimer: This content is for educational purposes only and does not constitute medical advice. Individual results may vary. Always consult with your healthcare provider about your specific condition and treatment options.
Key Points
✓ Interventional pain management is a specialized medical discipline that diagnoses and treats chronic pain using targeted, minimally invasive procedures rather than long-term opioids or major surgery.
✓ The most common conditions treated include herniated discs, sciatica, facet joint pain, spinal stenosis, sacroiliac joint dysfunction, and neuropathic pain.
✓ Common procedures include epidural steroid injections, nerve blocks, radiofrequency ablation (RFA), spinal cord stimulation (SCS), and facet joint injections.
✓ A 2024 review in Cell Reports Medicine confirmed that combining interventional, behavioral, and physical therapies produces the best long-term outcomes for chronic pain.
✓ For patients with a correctable structural cause, minimally invasive spine surgery such as Deuk Laser Disc Repair® at Deuk Spine Institute may offer a permanent cure rather than ongoing pain management
✓ Deuk Spine Institute offers a free MRI review to help patients understand their diagnosis and identify the best path to becoming pain free.
Living Beyond Chronic Pain
Chronic pain is one of the most widespread and undertreated health conditions in the United States. According to the World Health Organization, low back pain alone is the leading cause of disability worldwide, affecting an estimated 619 million people globally as of 2020. 1 In the United States, more than 50 million Americans live with chronic pain, with roughly 20 million experiencing high-impact chronic pain that limits work, social life, and basic daily activities. Back pain and neck pain are consistently among the leading causes of disability and lost productivity in the country.
If you have been struggling with pain that has not responded to rest, physical therapy, or anti-inflammatory medications, your physician may have recommended an interventional pain management specialist. But what does that term actually mean? What do these doctors do, what techniques do they use, and when does their approach make more sense than spine surgery?
This comprehensive guide answers those questions using the expertise of the Deuk Spine Institute team and the latest published medical research. Whether you are newly diagnosed or have been managing pain for years, this resource is designed to help you make informed decisions about your care.
What Is Interventional Pain Management?
Interventional pain management is a discipline of medicine devoted to the diagnosis and treatment of pain-related disorders, principally through the application of interventional techniques in managing subacute, chronic, persistent, and intractable pain, independently or in conjunction with other modalities of treatment.
In practical terms, an interventional pain physician uses procedures such as injections, nerve blocks, and implantable devices to interrupt pain signals before they reach the brain. The goal is not merely to mask pain with medication, but to identify the precise anatomical structure generating the pain and treat it directly.
Unlike general pain management, which may rely heavily on prescription medications, interventional pain management emphasizes an accurate diagnosis before treatment begins. A detailed evaluation and targeted diagnostic procedures help the physician identify the specific disc, nerve, facet joint, or soft tissue that is the pain generator. Once identified, the appropriate interventional technique is deployed to reduce or eliminate the pain signal at its source.
A major 2024 review published in Cell Reports Medicine by researchers at NYU Grossman School of Medicine confirmed that the modern standard of care for chronic pain involves a multimodal approach combining pharmacological, interventional, behavioral, and physical therapies. 2This research underscores what leading pain physicians have long advocated: no single treatment works for every patient, and a thoughtful combination of strategies consistently produces the best outcomes.
Who Are Interventional Pain Management Doctors?
Interventional pain management specialists come from several medical backgrounds, and their training pathways reflect the complex, multidisciplinary nature of chronic pain care.
The majority of interventional pain physicians have completed a five-year residency in anesthesiology, followed by a one-year fellowship specifically in pain medicine. Physicians trained in physical medicine and rehabilitation (physiatry) can also enter this specialty through a dedicated fellowship. In some cases, neurologists and sports medicine specialists choose to subspecialize in interventional pain management as well.
What distinguishes true interventional specialists from general practitioners is their procedural training. Fellowship-trained doctors have hands-on experience with image-guided injections, nerve ablation techniques, spinal cord stimulation, and other advanced procedures that require years of supervised training to master safely.

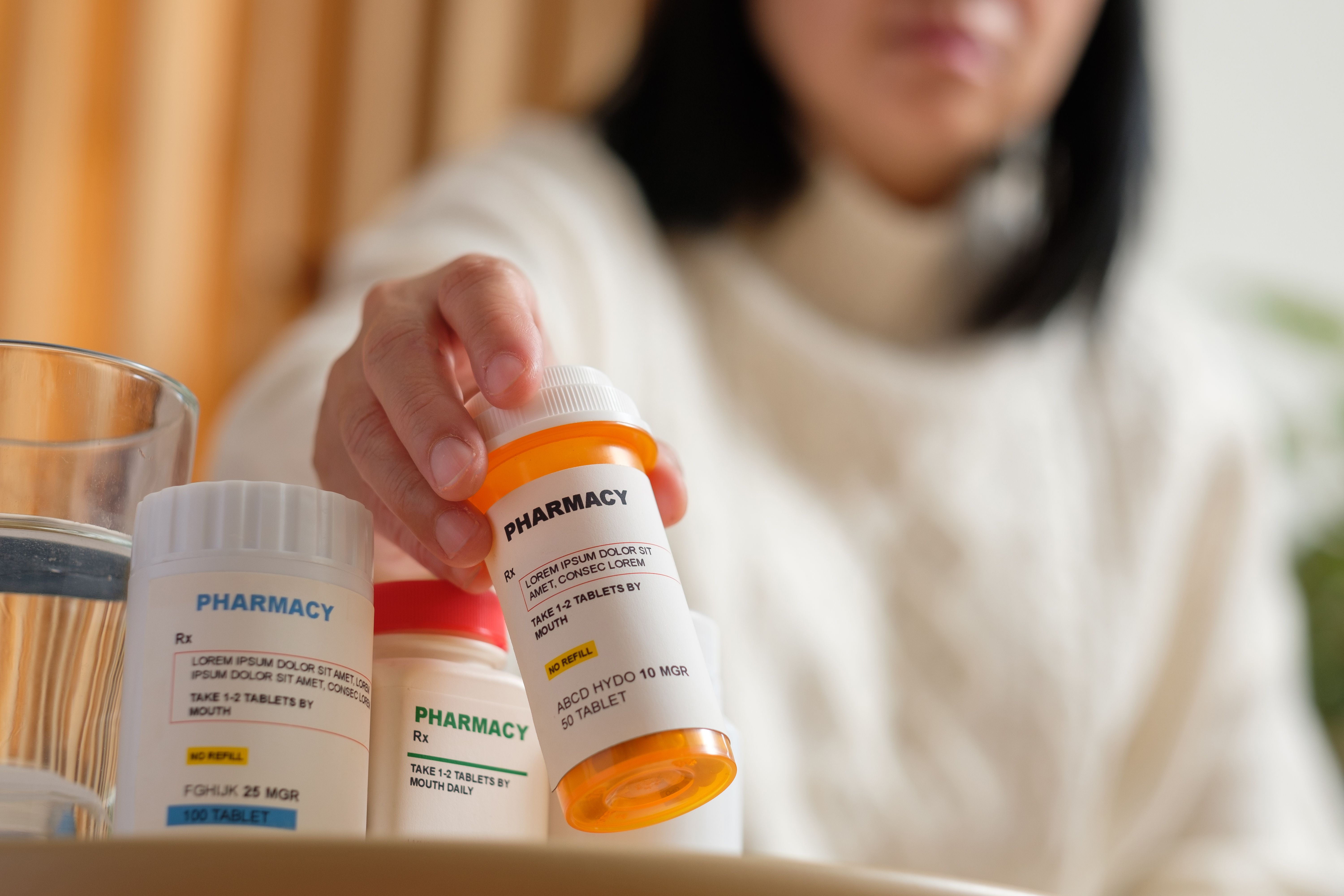
It is also important to understand the difference between an interventional pain specialist and a medical pain management specialist. Medical pain management doctors, such as primary care physicians or internists, primarily manage chronic conditions with medications including opioids. An interventional specialist, by contrast, uses procedures to treat the structural source of pain. Patients who have been prescribed long-term pain medications by a general physician but have never had a procedural evaluation may benefit significantly from an interventional consultation.
What Conditions Does Interventional Pain Management Treat?
Interventional pain management physicians treat a wide spectrum of painful conditions, the majority of which originate in the spine. The most common diagnoses include:
- Herniated or bulging discs: A disc that presses on an adjacent nerve root, producing arm pain (cervical radiculopathy) or leg pain (lumbar radiculopathy) in addition to neck or back pain.
- Sciatica: Radiating pain, numbness, or tingling that travels from the lower back down the buttock and into the leg, typically caused by compression of the sciatic nerve.
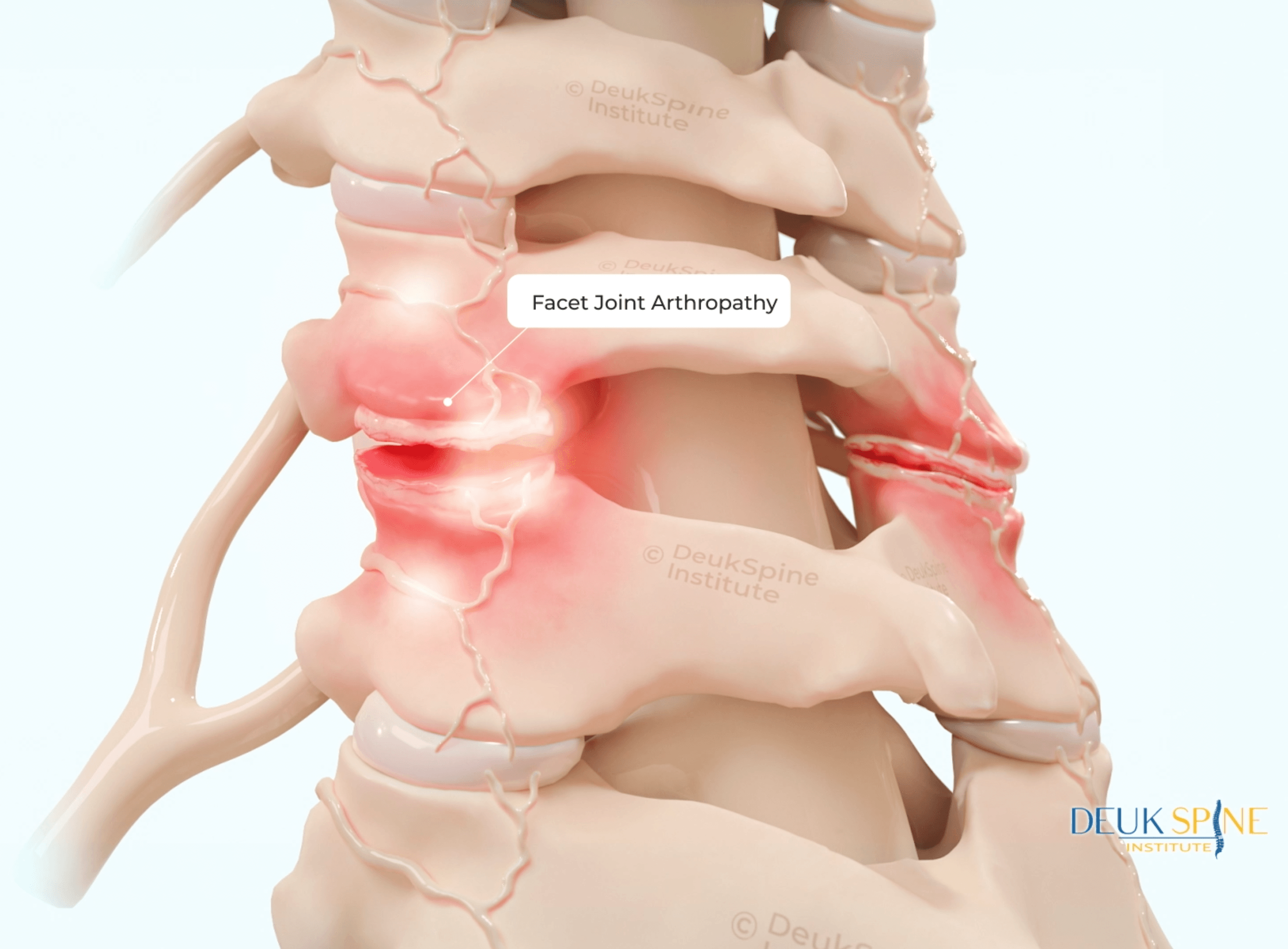
- Facet joint pain: Degenerative changes in the small joints between vertebrae that can cause localized or referred spinal pain, often worsened by extension movements.
- Spinal stenosis: Narrowing of the spinal canal that compresses the spinal cord or nerve roots, producing pain, weakness, and difficulty walking.
- Degenerative disc disease: Age-related breakdown of the intervertebral discs that causes chronic axial back or neck pain, often combined with radicular symptoms.
- Sacroiliac joint dysfunction: Pain originating from the joint that connects the sacrum to the pelvis, frequently misdiagnosed as lumbar disc disease.
- Complex regional pain syndrome (CRPS): A chronic pain condition most commonly affecting an arm or leg after injury or surgery, characterized by disproportionate pain, swelling, and autonomic changes.
- Neuropathic pain: Pain arising from nerve damage or abnormal nerve function, which often does not respond well to standard over-the-counter medications.
- Post-surgical pain: Ongoing pain following spine surgery, including failed back surgery syndrome, which affects an estimated 10 to 40 percent of patients who undergo lumbar spine procedures.
Neck and back pain together account for the vast majority of cases managed by interventional pain physicians. If chronic neck or back pain has not responded to conservative treatment over a period of weeks to months, an interventional evaluation is a well-supported next step.
Common Interventional Pain Management Techniques
Interventional pain management physicians have a broad and growing toolkit. A 2025 systematic review and network meta-analysis published in The BMJ evaluated the comparative effectiveness of common interventional procedures for chronic non-cancer spine pain. And found that targeted, image-guided approaches consistently outperform non-specific treatments for both short- and long-term pain relief. 3 Rather than applying one-size-fits-all treatments, specialists select procedures based on precise diagnosis, patient anatomy, and treatment history.
Epidural Steroid Injections
Epidural steroid injections (ESIs) are among the most commonly performed interventional pain procedures in the United States. A corticosteroid medication is delivered into the epidural space surrounding the spinal cord and nerve roots. The steroid reduces inflammation around compressed or irritated nerves, providing pain relief that may last from several weeks to several months.
ESIs are frequently used for sciatica, herniated disc radiculopathy, and spinal stenosis. They can function as standalone treatments or as part of a broader rehabilitation plan incorporating physical therapy and exercise programming.
Nerve Blocks
Nerve blocks interrupt pain signal transmission by delivering a local anesthetic, steroid, or longer-acting agent near a specific nerve or nerve group. Depending on the condition, nerve blocks may be applied as short-acting diagnostic tools or as therapeutic treatments with longer duration.
Selective nerve root blocks and medial branch blocks are commonly used both diagnostically and therapeutically. When a nerve block provides meaningful temporary relief, it confirms the treated nerve as the primary pain generator and guides the selection of the next, more definitive treatment.
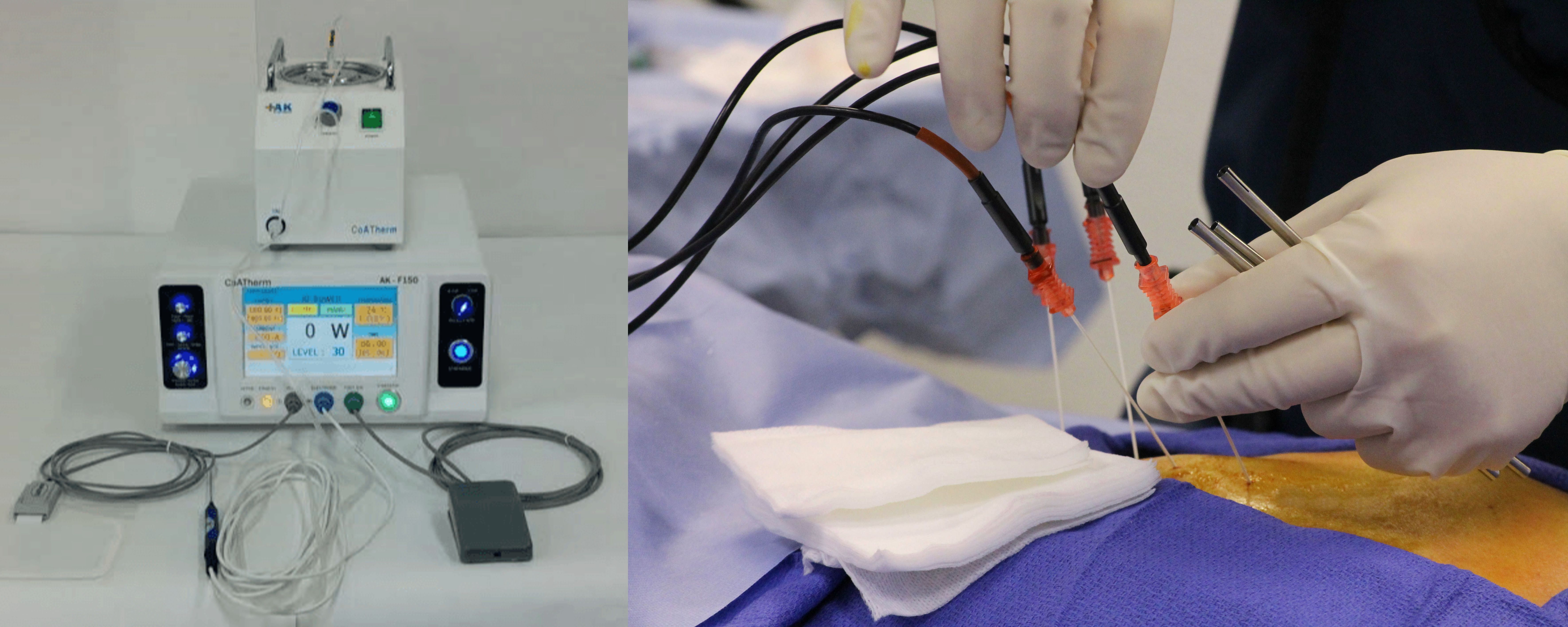
Radiofrequency Ablation (RFA)
Radiofrequency ablation uses heat generated by radio waves to selectively disable the small nerves transmitting pain signals from arthritic facet joints or the sacroiliac joint. After a successful diagnostic medial branch block confirms the target nerve, the physician applies radiofrequency energy to ablate the nerve, producing pain relief that typically lasts 12 months or longer.4
A bibliometric analysis examining pain management research from 2000 to 2024 identified radiofrequency ablation as one of the fastest-growing areas in the specialty, with a growing body of high-quality evidence supporting its use for chronic musculoskeletal pain. Pain Physician and Pain Medicine were ranked as the leading journals in this expanding field.
Spinal Cord Stimulation (SCS)
Spinal cord stimulation involves implanting a small pulse generator that delivers low-level electrical impulses to the spinal cord, altering the way pain signals are perceived by the brain. SCS is typically reserved for patients who have not achieved adequate relief from other treatments, including surgery. A 2025 study published in the Journal of Clinical Medicine found that closed-loop spinal cord stimulation significantly outperformed open-loop SCS in reducing pain at 36 months, with a higher proportion of patients achieving at least 50 percent pain reduction. 5 These advances are elevating SCS from a last-resort option toward a more broadly accessible and highly effective long-term therapy for appropriate candidates.

Facet Joint Injections
Facet joints are paired joints at each spinal level that allow the spine to bend and twist. When these joints become inflamed or arthritic due to age or injury, they can generate significant localized and referred pain. Facet joint injections deliver corticosteroid medication directly into or adjacent to the affected joint under fluoroscopic or ultrasound guidance.
Facet injections serve both as diagnostic tools and therapeutic treatments. When a specific joint is confirmed as the pain source, injections combined with physical therapy can provide months of meaningful relief.
Regenerative Medicine: PRP and Stem Cell Therapies
One of the most rapidly evolving areas in interventional pain management is regenerative medicine, which leverages the body's own healing biology to repair damaged tissue. Platelet-rich plasma (PRP) and stem cell injections are being actively studied for degenerated discs, facet arthritis, and soft tissue injuries. A 2025 comprehensive guideline update from the American Society of Interventional Pain Physicians compiled 19 evidence-based recommendations on regenerative therapies for chronic low back pain, with all 19 recommendations achieving 100 percent consensus across a 33-member expert panel. 6 This represents a meaningful step toward formalizing regenerative interventions within mainstream practice.
The Multidisciplinary Approach to Pain Management
One of the defining characteristics of high-quality interventional pain management is the multidisciplinary model of care. Rather than relying on a single treatment, the best programs coordinate treatment across multiple specialties to address every dimension of a patient's pain experience.
A comprehensive pain management program typically coordinates care across the following areas:
- Physical therapy and rehabilitation to restore strength, flexibility, and functional movement
- Psychological support including cognitive behavioral therapy (CBT), which is a proven evidence-based intervention for chronic pain
- Nutritional and lifestyle guidance, since anti-inflammatory dietary patterns and regular aerobic exercise have documented pain-reducing effects
- Interventional procedures to address the structural or neurological source of pain
- Surgical consultation when imaging reveals a correctable problem that requires a more definitive solution
A long-term prospective study published in the Journal of Clinical Medicine (2025) followed patients with chronic spinal pain over four years following interventional procedures. 7 Patients who consistently participated in physical therapy alongside their interventional treatments had significantly better outcomes in pain intensity, disability scores, and quality of life compared to those who did not. This confirms what experienced pain physicians have consistently observed: interventional procedures deliver their best results as part of a coordinated, patient-centered treatment plan.
Find out how Dr. Deuk can permanently ease your back pain. Starting with a quick, 10-minute free virtual consultation.

Notable Interventional Pain Management Specialists
Interventional pain management is a field defined by the expertise and dedication of its physicians. Below are several recognized leaders in this specialty who exemplify the high standard of care patients deserve.
1. Dr. Andrew H. Morchower

Dr. Andrew H. Morchower is a fellowship-trained interventional spine and pain management specialist who is board-certified in Physical Medicine and Rehabilitation. He hails from Dallas, Texas, and completed his interventional spine and pain fellowship at Pennsylvania Orthopaedic and Spine Specialists.
Dr. Morchower finished his residency in Physical Medicine and Rehabilitation at the University of Texas Southwestern Medical Center. He earned his medical degree and a master's degree in public health from Tulane University School of Medicine in New Orleans. He has lectured on pain management topics both nationally and internationally and is known for his approach that draws on both physical medicine and interventional training to create individualized treatment plans for each patient.
2. Dr. Maulik Bhalani, MD

Dr. Maulik Bhalani is the founder and CEO of Florida Pain Medicine, a multi-location interventional spine and pain management facility with offices across the Tampa Bay region and Central Florida. He is double board-certified in interventional pain medicine and physical medicine and rehabilitation by the American Board of Physical Medicine and Rehabilitation and the American Board of Medical Specialties.
Dr. Bhalani earned his medical degree from Creighton University in Omaha, Nebraska, and completed a physical medicine and rehabilitation residency at the University of South Florida, where he served as chief resident. He then completed a prestigious two-year interventional pain medicine fellowship at USF, serving as chief fellow. His training also included a transitional internship and partial anesthesiology training at the University of Maryland Medical Systems in Baltimore.
Dr. Bhalani currently serves as clinical associate professor and faculty for the University of South Florida Health ACGME Pain Medicine Fellowship and the Department of Neurology, making Florida Pain Medicine a core rotation site for pain medicine fellows and physical medicine and rehabilitation residents. He is Vice President of the Florida Society of Interventional Pain Physicians (FSIPP) and attends national conferences each year to bring the latest techniques directly to his patients.
Interventional Pain Management vs. Spine Surgery: Which Is Right for You?
A question patients frequently ask is: when is pain management the appropriate choice, and when should surgery be considered?
Interventional pain management is generally the right first step when:
- Pain is moderate and has not fully responded to conservative care including rest, anti-inflammatories, and physical therapy
- Imaging shows nerve irritation or inflammation that may respond to targeted injections or nerve blocks
- The goal is to delay or avoid surgery while managing symptoms and building function
- Procedures are being used as diagnostic tools to confirm the precise pain source before committing to surgery
Surgery becomes the appropriate conversation when:
- Imaging reveals a structural problem such as a herniated disc, spinal stenosis, or significant disc degeneration causing nerve compression
- Interventional treatments are providing progressively shorter and less effective relief over time
- Neurological symptoms are present, including progressive muscle weakness, numbness, or loss of bladder or bowel control
- The structural problem is correctable with a minimally invasive procedure that addresses the root cause rather than the symptoms
At Deuk Spine Institute, interventional pain management and surgical expertise work together under one roof. Pain management procedures often serve as both treatment and diagnosis, helping to clarify whether a patient is a candidate for surgery and ensuring that surgical decisions are based on the most complete picture possible.
Deuk Laser Disc Repair®, the signature minimally invasive procedure developed by Dr. Ara Deukmedjian, has a 95 percent success rate with no surgical complications across thousands of procedures. For appropriately selected patients, it offers a permanent cure rather than a cycle of ongoing treatments.
Dr. Ara Deukmedjian: Bridging Pain Management and Surgical Expertise at Deuk Spine Institute

Dr. Ara Deukmedjian, known to his patients and colleagues as Dr. Deuk, is a world-renowned board-certified neurosurgeon and the founder of Deuk Spine Institute in Florida. He is a pioneer in minimally invasive, laser, and endoscopic spine surgery for the treatment of neck, back, and thoracic pain, and has performed thousands of successful procedures with an unmatched safety record.
Dr. Deuk is a member of the Congress of Neurological Surgeons (CNS) and the American Association of Neurological Surgeons (AANS). He has served as Surgery Department Chair at Parrish Medical Center and has received the Patients Choice Award for multiple consecutive years.
His signature procedure, Deuk Laser Disc Repair®, is the most advanced minimally invasive laser spine surgery in the world. Unlike traditional open spine surgery or total disc replacement, Deuk Laser Disc Repair® preserves disc anatomy, eliminates the pain source directly, and has demonstrated a 95 percent success rate with zero surgical complications. It is a genuine alternative for patients who have been told their only option is major surgery.
Dr. Deukmedjian personally reviews each patient's MRI during the free Deuk Spine Exam, ensuring that every recommendation is grounded in accurate diagnosis rather than assumptions or incomplete imaging interpretation. At Deuk Spine Institute, patients benefit from the full continuum of spine and pain care, from the most conservative interventional options to the most advanced surgical solutions.
When Should You See an Interventional Pain Management Doctor?
The utilization of interventional pain management in the Medicare population has shifted significantly in recent years. A 2025 analysis published in Pain Physician examined trends from 2019 to 2024 and found notable changes in procedure volume and access patterns, reinforcing the importance of patients proactively seeking specialized evaluation rather than waiting for a referral. 8 You should consider a consultation with an interventional pain management specialist if any of the following apply:
- Your back or neck pain has persisted for more than 6 to 12 weeks despite conservative treatment
- Over-the-counter medications, physical therapy, or rest have not provided lasting relief
- Pain is significantly affecting your ability to work, sleep, or carry out daily activities
- You are experiencing radiating pain, numbness, or tingling into an arm or leg
- Your primary care physician or a specialist has recommended a formal pain management evaluation
In most cases, you do not need a referral to see an interventional pain specialist, though your primary care doctor can help facilitate the process by sharing relevant imaging and medical records.
How to Prepare for Your First Appointment
Arriving well prepared helps your pain physician make the most accurate diagnosis in the shortest time possible. Before your appointment, consider the following:
- Keep a pain journal for one to two weeks noting when pain occurs, what makes it better or worse, where it radiates, and how it affects your daily life
- Gather all recent imaging including MRI scans, CT scans, and X-rays. Bring hard copies if digital transfer has not been arranged in advance
- List all current medications, supplements, and over-the-counter drugs
- Write down previous treatments including injections, surgeries, and physical therapy programs, along with how well each worked
- Prepare a list of questions. Common ones include: What is causing my pain? What procedures do you recommend and why? How long will relief last? What are the risks?
Confirming that your physician has completed a fellowship specifically in pain management is an important step. The interventional pain field advances rapidly, and fellowship-trained specialists have access to cutting-edge techniques and evidence-based protocols that general practitioners do not.
Take the First Step Toward a Pain-Free Life
Chronic neck and back pain do not have to define your daily experience. Whether your path forward involves interventional pain management procedures, minimally invasive spine surgery, or a thoughtful combination of both, Deuk Spine Institute has the expertise, the technology, and the multidisciplinary team to help you find lasting relief.
Schedule your Free MRI Review and Deuk Spine Exam today. Dr. Ara Deukmedjian and the Deuk Spine Institute team will personally review your imaging, assess your symptoms, and provide you with an honest diagnosis and a clear set of treatment recommendations. Call 1-800-FIX-MY-BACK or request your consultation online.
Frequently Asked Questions
Q: Is interventional pain management the same as seeing a doctor who prescribes opioids?
A: No. Interventional pain management is specifically focused on procedures rather than long-term opioid prescribing. A medical pain management specialist, such as a primary care physician managing a patient with a chronic pain condition, may prescribe opioids as part of their practice. An interventional specialist, by contrast, uses injections, nerve blocks, ablations, and implantable devices to treat the source of pain directly. Opioids may play a short-term role in some patients' care, but they are not the primary tool of an interventional practice.
Q: How many procedures will I need?
A: This depends on the underlying cause of your pain, the procedure performed, and how your body responds to treatment. Some patients achieve sustained relief after a single injection combined with physical therapy. Others benefit from a series of procedures over several months. Radiofrequency ablation, for example, typically requires a two-step process: a diagnostic nerve block to confirm the target, followed by the ablation itself. Your physician will outline a realistic treatment plan during your initial consultation.
Q: What is the difference between an interventional pain doctor and a spine surgeon?
A: An interventional pain management physician focuses on non-surgical procedures to manage pain and improve function. A spine surgeon evaluates whether a structural problem in the spine can and should be corrected operatively. Many patients benefit from seeing both specialists, particularly at a comprehensive practice like Deuk Spine Institute where pain management and surgical expertise are coordinated under one roof. In many cases, interventional procedures help confirm the exact pain source and establish clearer surgical candidacy.
Q: Can interventional pain management provide permanent relief?
A: Some procedures provide long-lasting or permanent relief, particularly when the underlying cause is a well-defined structural problem that responds predictably to treatment. Radiofrequency ablation typically provides 12 or more months of relief, though nerves can regenerate over time and symptoms may eventually return. For patients with a structurally correctable problem, minimally invasive spine surgery such as Deuk Laser Disc Repair may offer a permanent cure. The right answer depends entirely on your specific diagnosis, which is why a thorough evaluation is always the first step.
Sources
- World Health Organization (2023). Low Back Pain Fact Sheet.
- Wang X et al. (2024). Clinical pain management: Current practice and recent innovations. Cell Reports Medicine. PMC11513809.
- Wang et al. (2025). Common interventional procedures for chronic non-cancer spine pain: a systematic review and network meta-analysis. BMJ. https://doi.org/10.1136/bmj-2024-079971
- Artuç, S. E., & Kamacı, G. K. (2025). Radiofrequency ablation for musculoskeletal pain: A bibliometric analysis of global research trends (2000–2024). Pain Physician, 28(Supplement 7), S157–S168.https://pubmed.ncbi.nlm.nih.gov/41481873/
- Journal of Clinical Medicine (2025). Innovations in Spinal Cord Stimulation: Closed-Loop vs. Open-Loop SCS.
- Manchikanti et al. (2025). Comprehensive Evidence-Based Guidelines for Regenerative Therapies in Chronic Low Back Pain: 2025 Update. Pain Physician. PMID: 41481869.
- Baroncini A et al. (2025). Long-Term Follow-Up of Spinal Interventional Pain Procedures and Physical Therapy Compliance. Journal of Clinical Medicine.
- Manchikanti et al. (2025). Updated Analysis of Decline of Interventional Pain Management Utilization in Medicare Beneficiaries 2019-2024. Pain Physician. PMID: 41481870.